Learn the Ankle replacement-Star ankle replacement (revision of mensical component) surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Ankle replacement-Star ankle replacement (revision of mensical component) surgical procedure.
The polyethylene bearing of a mobile bearing ankle replacement may fracture, wear or dislocate.
If this happens, the whole ankle replacement may need to be revised, or just the meniscal bearing – mindful of the fact that some wear may also have occurred to the metal surfaces of talar and tibial components.
It is important to identify any precipitating factors which may have caused the meniscus to fail (such as ankle instability or component malalignment) and to correct these at the same time as revising the bearing.
For those undertaking ankle replacement surgery the ability to identify and deal with its potential complications (both in the short and longer term ) should be a consideration.
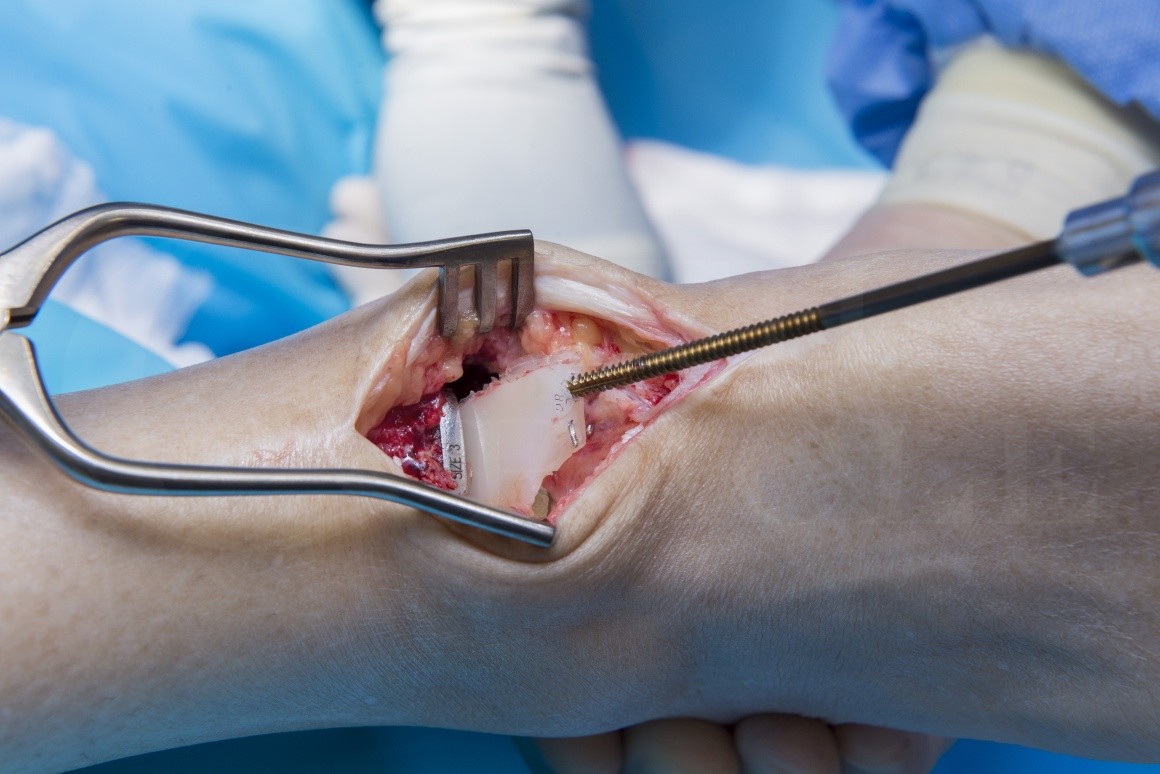
The following operation demonstrates my technique for managing the isolated failure of a meniscal component of a STAR ankle replacement , one of the implants with the longest track record.

INDICATIONS:
The mobile bearing may fail due to wear or fracture(age related), dislocation (secondary to trauma or instability) or a combination of these factors.
SYMPTOMS & ASSESSMENT:
The patient may feel progressive pain, swelling or instability of the ankle, or failure may be detected on routine follow up xrays.
INVESTIGATION:
The patient must be carefully examined, to check stability and alignment of the joint.
Plain xrays should be carefully studied, looking to see where the bearing or its components lie, checking the alignment and fixation of the components, and looking for causative factors such as impinging new bone formation, which may have caused maltracking.
Routine blood tests looking for raised inflammatory markers and infection should be performed.
Patients should have a spiral CT scan performed, looking for cyst new bone formation, signs of loosening, and looking for cyst formation which may occur secondary to polyethylene wear.
OPERATIVE ALTERNATIVES:
The surgeon should always consider whether other procedures need to be performed at the time of bearing exchange.These may include stabilisation procedures, excision of impinging intra-articular scar or osteophytes, or grafting of cysts.
If there is visble wear of the metal surfaces, or major cyst formation, then revision ankle replacement or conversion to fusion may be needed. Sometimes the decision whether to revise or fuse can only be made at surgery, and the surgeon must be equipped and ready for either of these eventualities.
NON-OPERATIVE ALTERNATIVES:
Non-operative treatment should only be undertaken for patients who are too frail for surgery. in such cases a light ankle brace may help stabilise an unstable ankle, and provide some symptomatic relief.
CONTRAINDICATIONS:
Replacing the mobile bearing is contra-indicated in patients with infection, and should be postponed if there is adjacent skin infection.
The presence of loosening, malposition,large cysts,or wear of the metal surfaces may all be contra-indications , and point to the need for ankle joint revision or fusion.

All the equipment needed for a revision ankle replacement (including revision extra thick bearings) should be available.
If there is a possibility of proceeding to fusion, a suitable nail or plate set and bank bone (or consent to take iliac crest bone) should be ordered.
An image intensifier is mandatory.
The patient is positioned prone, a touniquet applied and the leg prepped according to hospital protocols.
Antibiotics should be withheld until any biopsy samples have been taken.

The foot should be immobilised in a cast or boot to protect the wound for 2 weeks.
The patient may bear weight through the cast boot during this period.
Anticoagulation is administered throughout the period of immobilisation if local protocols dictate.
Provided the wound has healed at 2 weeks, the sutures can be removed and the patient mobilised with a light ankle brace for security.
the cast /boot is retained until the wound is dry and healed.
On removal of the cast/boot the patient should be taught active and passive dorsiflexion exercises.
Annual review with radiographs is mandatory after bearing replacement, in case irregularity of the metal surface (caused during the period that the bearing has been deficient) causes early repeat failure.

It is not possible to define the incidence of bearing failure, as many studies and some long-standing registries do not record failure of the bearing, nor count replacement of the bearing as a revision.
It is similarly not possible to define the longevity of the bearing replacement procedures , although increasingly registries – including the UK National joint registry- are recording survival of ankles after bearing replacement.
Surgeons and patients should be aware that the bearing may suffer early failure, and patients having this procedure should be carefully followed up with regular xray checks for life.
Reference
- orthoracle.com















