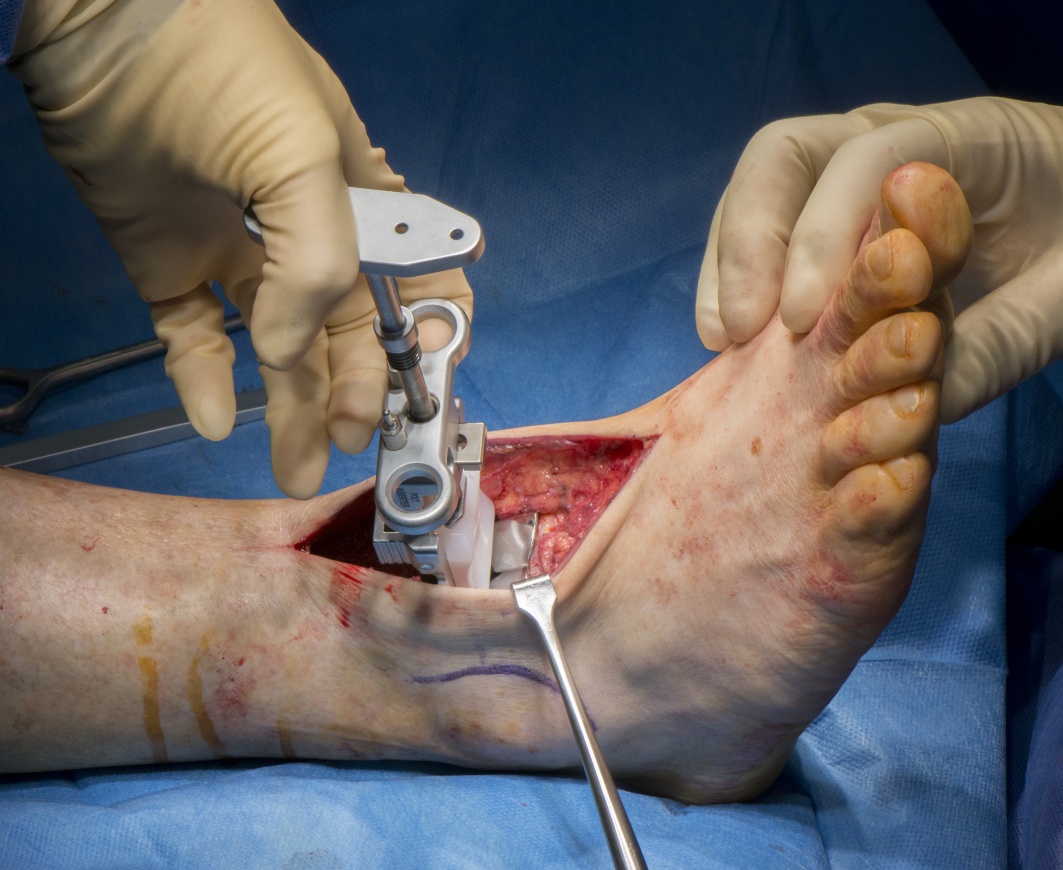
Learn the Ankle replacement-Wright Infinity ankle replacement surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Ankle replacement-Wright Infinity ankle replacement surgical procedure.
Total Ankle replacements have been implanted for the treatment of arthritic conditions of the ankle for a few decades now. The design and biomechanics of these early implants was at best rudimentary and were manufactured on the premise that the ankle is a monoaxial joint capable of movement only in the sagittal plane. It did not allow for translational or rotational movements of the ankle that is now known to occur in human ankles. These were simple two component assemblies that articulated against each other and failed either due to lack of osseointegration or excessive wear
Subsequent generations of implants used more modern ideology to create metal components for the tibia and talus with intervening ultra high molecular weight polyethylene acting either as a spacer when fixed or as a meniscus engaging in mobile bearing functions. These proved to be much more successful both in terms of function and of survivorship. The Wright Infinity ankle replacement is one of the latest evolutions of ankle replacement.
The use of the Prophecy cutting jigs are a unique feature of the Wright Infinity Ankle Replacement. This requires a CT scan of the lower limb in question (using a specific protocol ) to enable 3D technology to create these unique jigs. The software uses specific anatomic high points on the tibia and talus including prominences osteophytes and peaks and troughs to create a Wright Infinity jig that will sit on the respective bones fitting into these high points (the so called ‘sweet spot’ where the jig fits perfectly without a toggle). The software also creates an accurate model of the distal tibia and the talus which are sterilisable so that the jig can be fitted onto these anatomically perfect models to assess and practice the orientation of these jigs when fitted on to the actual patients ankle bones on table. Thus at least two copies of these bone models are available sterilised to use for practice on table
Readers will also find the following associated techniques of interest:
Ankle replacement-Wright Prophecy
Ankle Replacement-BOX total ankle replacement (MatOrtho)
Ankle replacement-Revision using Wright Invision Ankle replacement system
Ankle replacement-Star ankle replacement (revision of mensical component)
Ankle Replacement -De Puy Mobility

INDICATIONS:
Post traumatic osteoarthritis of the ankle remains the most frequent indication for ankle arthroplasty. This usually occurs after fracture subluxations/dislocations associated wth significant chondral damage leading to concentric osteoarthritic changes. sometimes massive chondrolysis leads to a similar picture
Pantalar arthritis or arthritis in more than 2 joints in the hind/mid foot is a compelling indication as the joint replacement seeks to preserve some movement in the hindfot whilst needing to fuse the joints that cant be replaced. This is usually a combination of ankle subtalar chopart or tarsometatarsal joint arthritis. The other indications are arthritis due to ligament deficienccy usually associated with some deformity. the use of ankle arthroplasty in the presence of deformity is still being debated as there is some published evidence that the replacement fails in the direction of the deformity i.e a varus arthritis of an ankle when replaced will fail in varus. however the use of designs such as the InBone seems to mitigate against this possibiity by using intramedullary stems in the tibia.However the definitive evidence is still lacking.
Bilateral ankle arthritis is thought to be a good indication for replacing atleast one of the ankles to ensure that gait is not significantly altered.
It is however clear that the use of ankle replacement for arthritic conditions of the ankle is gaining traction worldwide
SYMPTOMS & ASSESSMENT:
Symptoms: Patients complain universally of pain particularly when weight bearing.Sometimes there is associated swelling with symptoms of instabiity if there is ligament deficiency. There is often stiffness particularly after a period of inactivity such as on waking up or being seated for a period of time. The patient often describes needing to ‘walk it off’. As the arthritic changes worsen, stifffness increases often in dorsiflexion but also in plantarflexion. Achilles tendon tightness is very common in these patients and lengthening of the achilles tendon is the commonest adjuvant procedure that is performed alongside the ankle replacement.Night pain is uncommon but can be present in cases where there are severe mechanical symptoms with grating clicking or crepitus causing severe pain. The girth of the ankle is often increased and may affect footwear
Associated arthritis in neighbouring joints will cause corresponding symptoms.
INVESTIGATION: Standing anteroposterior and lateral radographs are essential to assess the talocrural geometry and alignment. In addition Saltzmann views include the oscalcis talus and tibia to give an excellent appraisal of the coronal alignment of the hindfoot. This is essential to assess the overall alignment of the hindfoot and ankle not only to accurately position implants but also to plan adjuvant procedures such as calcaneal osteotomy or subtalar fusion to realign the hindfoot.
The use of the Prophecy cutting jigs are a unique feature of the Wright Infinity Ankle Replacement. This requires a CT scan of the lower limb in question with a specific protocol to enable the 3D technology to create these jigs. The software uses specific anatomic high points on the tibia and talus including prominences osteophytes and peaks and troughs to create a Wright Infinity jig that will sit on the respective bones fitting into these high points (the so called ‘sweet spot’ where the jig fits perfectly without a toggle). The software also creates an accurate model of the distal tibia and the talus which are sterilisable so that the jig can be fitted onto these anatomically perfect models to assess and practice the orientation of these jigs when fitted on to the actual patients ankle bones on table. Thus at least two copies of these bone models are available sterilised to use for practice on table. It is therefore essential that this special CT protocol is utilised to create these jigs. It requires the radiology CT staff to familiarise themselves with the protocol in order that appropriate cuts are made and the correct images are reformatted to generate the 3D capability to create the jigs. Once these are generated they are sent off to the 3D lab where a report highlighting the salient features of the specific ankle is sent to the surgeon along with graphic images of the jigs for a formal sign off after assessing deformity and high points on the ankle. The ankle replacement operation then requires to be scheduled within 6 weeks of manufacture of the jigs to avoid any change in the profile of the ankle if the procedure was delayed.
Advantages of the implant system:
The Infinity TAR has several unique features to its design. It has a highly polished resurfacing talar component with no flanges on its sides allowing the operating surgeon to asses its position on the talus accurately by means of fluoroscopy. It is a pressfit design. It can be interchanged with its parent design prosthesis the InBone talar component which is implanted with a flat cut only and with no chamfer cuts, which is especially useful in certain anatomic aberrations such as a flat top talus. Its inherent sulcus geometry gives it coronal stability which is also useful as it relies less on surounding soft tissue for its stability. It has two anterior pegs for anchorage onto the talus.
The tibial tray design is of low profie and is made of a titanium alloy. It has 3 pegs which are angled backwards so that it can be impactd axially into the tibial surface. It requires the same standard resection thickness for all sizes. It comes with a long option to allow for a longer AP length of the taus without further bone resection.
The spacer is made of UHMWPE and is a fixed bearing being firmly secured into lace with a pressfit plunger mechanism on to rails on the tibial tray.
Perhaps the biggest advantage of this system is the ability to predictably position implants with a degree of acuracy that is hard to achieve with any other system. This can be done by using the PROPHECY system which is the preoperative nagivation system that creates cutting blocks customised to each patient.
OPERATIVE ALTERNATIVES: The obvious alternative is an arthrodoesis.
Arthroscopy in early and moderate osteoarthritis
Arthodiastasis is controvertialin moderate arthritis
Supramalleolar osteotomy in selected cases
NON-OPERATIVE ALTERNATIVES:
Analgesia, Intra-articular injection, life style modification, orthoses etc
CONTRAINDICATIONS:
severe deformity, severe osteonecrosis, severe osteopenia, previous arthrodoesis, charcot arthropathy, peripheral ischemic disease, actve sepsis or previous history of septic arthritis or osteomyelitis in the immediate vicinity of the ankle

The preoperative WHO meeting should confirm the availability of implants and their sterility. The nature of the operation and the side of surgery should be crosschecked with surgeon patient and theatre staff.
Radiographs should be appropriately displayed in theatre for referencing during the procedure.
The operation can be done under general anaesthesia in conjunction with an ankle block or under regional anaesthesia such as a spinal anaesthetic or a popliteal block.Warn the anaesthetist that the procedure could exceed 2 hours especially if additional procedures are required
In the absence of any other additional procedures such as a gastrocnemius release or a primary tendoachilles lengthening, the patient is positioned supine on the table with a sandbag under the ipsilateral buttock so as to position the foot orthogonally, with the axis of the foot perpendicular to the coronal plane. Diathermy is needed to cauterize veins that will be encountered during the procedure.
Specific to the Prophecy system the following steps are mandatory to ensure that the right process is being followed
1. Read and reread the report from the 3D manufacturer to confirm deformity and sizes
2. Match patient number with case number to ensure the right blocks are being utilised for that specific patient
3. Confirm anatomic features such as osteophytes loose bodies bone voids and cysts to make sure patient is adequately consented for auxiliary procedures such as tendoachilles lengthening, bone graft harvest, additional kit availability such as for osteotomy of malleoli, subtalar fusion synthetic grafts soft tissue anchors etc

The patient is kept in hospital for one to two nights. During this time the limb is elevated and the plaster completed after 24 hours. Postoperative antibiotics are given and also Daltaparin prescribed for 4-6 weeks. The patient is taught to walk with crutches non weight bearing for anything between 2 to 4 weeks. If there is a slight gap between prosthesis and bone then early weight bearing is commenced bearing in mind that there is a small risk of loosening. However as the patient is in a walking plaster it is thought that it would aid in axial impaction of the prosthesis to reduce any gap and to promote osseointegration of the implant. If the patient has had other procedures such as Tendoachilles lengthening or fusion procedures then the plaster is kept on non weightbearing for at least 6 weeks
Patient is usually prescribed combinations of Codeine and paracetamol after the first 48 hours and is discouraged from taking anti-inflammatories for their negative osteogenic effects.
Patient is reviewed at 1 week for a change of cast to a synthetic cast and wound check.
After 2 – 4 weeks the plaster is removed and replaced with a pneumatic boot and physio therapy is commenced.
The patient is then reviewed at 6 and 12 weeks when radiographs are done to ensure good progress towards osseointegration and to watch out for signs of infection loosening etc. at 3 months the patient is advised to mobilise independently and to continue physiotherapy until discharge .

Reference
- orthoracle.com
































































