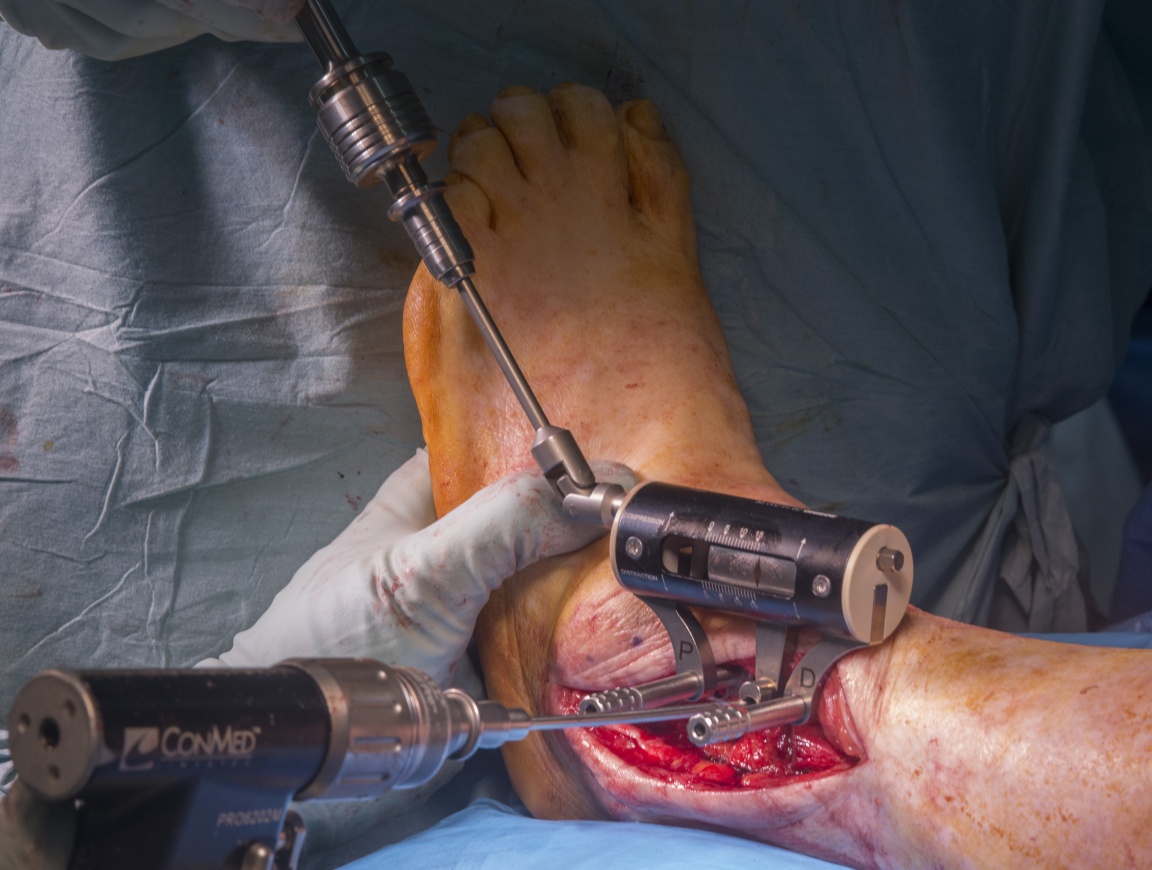
Learn the Ankle Fusion (arthrodesis): Trans-fibular approach using AnkleFix 40 plate (Zimmer-Biomet) surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Ankle Fusion (arthrodesis): Trans-fibular approach using AnkleFix 40 plate (Zimmer-Biomet) surgical procedure.
Ankle arthrodesis is an established treatment for painful, end-stage ankle arthritis. Over the last century, a number of operative techniques have been popularised, with modifications reflecting technological advances. These have ranged in methods of fixation from the Charnley external clamps through to all manner of crossed/parallel screw fixation techniques.
However, managing deformity, poor bone quality or bone loss remain difficult issues to resolve using traditional techniques. As a result, biomechanical studies into the properties of angle-stable devices such as blade plates and non-anatomic locking plates have found some mechanical advantages over screws in stabilising an ankle arthrodesis, thus potentially offering a solution. Therefore, in Sheffield, Mr Mark Davies and Mr Chris Blundell developed a new anatomically contoured, fixed angled lateral locking ankle arthrodesis plate – the Ankle Fix 4.0. Manufactured by ZimmerBiomet, we have successfully used this device for open ankle fusion surgery especially in more challenging clinical situations. The rationale behind the plate design was formed after both authors had gained experience using an inverted PHILOS plate. It was felt that a set of divergent screws within a low-profile talar section would offer a significant pull-out strength in cancellous bone and similarly that convergent screws in the tubular, cortical bone would provide robust tibial fixation. These screws were specifically designed to be 4.0 mm in size to allow clustering of the screws which contrasts with the larger, less versatile plate designs that were on the market at the time of design in 2009.
With limited literature on the wealth of new locking ankle fusion plates, the plate designers present these results and discuss their large series in the December 2017 issue of the journal Techniques in Foot and Ankle Surgery.

Indications
The indications for use of the Ankle Fix 4.0 lateral locking plate include:
1 End-stage arthrosis of the ankle joint, especially in the presence of deformity or osteopenia
2 Failed previous ankle arthrodesis (mal-union and non-union)
3 Tibio-crural bone loss (failed total ankle replacement, avascular necrosis) provided there is sufficient remaining bone stock in the body of the talus.
The Ankle Fix plate is a tool to combat the above challenges therefore, in my practice, it is used if an arthroscopic ankle fusion cannot deal with any of the above indications.
Symptoms & Examination
In all of the indications, pain is the most common symptom. However, when present, deformity may be equally as disabling especially if the patient is struggling to find stable, comfortable, corrective or accommodative footwear. Therefore, another intrusive symptom may be the instability with any associated pain or swelling.
Examination for all indications should include a careful appraisal of the soft tissue envelope. Specifically, the location of previous surgical scars will govern future surgical approaches, the presence or absence of pedal pulses will influence the ability of a fusion mass to heal and, any evidence of ongoing or previous infection may abort plans for further surgical intervention.
Assessment of any deformity requires consideration of all three planes of deformity. The deformity should be assessed for fixity and also the mobility of neighbouring joints, especially the subtalar and talo-navicular joint. Wherever possible, the subtalar joint should be preserved not only because fusing this joint adds significant morbidity, but also because a tibio-talo-calcaneal fusion is associated with poorer functional outcomes.
Investigation
In my practice, weight-bearing views in two planes of the ankle and an additional oblique view of the foot are mandatory as baseline imaging. In the case of a large coronal pane deformity it is particularly pertinent to fully assess the subtalar joint. When the subtalar joint is suspected of being symptomatic, a fluoroscopically guided arthrogram and local anaesthetic injection is helpful in isolating the source of symptoms. The reason for the arthrogram in this assessment is to determine any continuity of joint capsule between neighbouring joints as this can confound the results of the local anaesthetic infiltration.
CT is another useful investigation as this can assess neighbouring joint disease as well as determine remaining bone stock after previous surgeries. As a rule there should be approximately 2cm of remaining height of the body of the talus to accommodate the talar footprint of the Ankle Fix 4.0 plate.
Operative alternatives
In broad terms, ankle arthrodesis can be performed either by open or arthroscopic methods. Initial use of arthroscopic ankle fusion was confined to cases with minimal coronal plane deformity, but over time experienced enthusiasts of this technique have been more able to deal with larger deformities. Clearly, it has no role in revision surgery and it may be less effective in poor quality bone.
Open techniques using various numbers and positioning of screws have been the mainstay of ankle fusion procedures for decades. Some experienced enthusiasts have had success in dealing with large deformity and with bone loss and poor bone quality, but with an ageing population, these latter two issues have become more apposite. More people are presenting later in life with end-stage ankle arthrosis and after failed total ankle replacement necessitating alternative methods of fixation. Although Ilizarov techniques can be used to address these problems, these fine wire frames are not well-tolerated by patients.
Contraindications
Absolute contraindications for this technique include active Charcot arthropathy and the presence of either superficial or deep infection.
Non-operative intervention
Non-operative pharmaceutical measures may include judicious use of analgesics and anti-inflammatory medications (NSAIDs) and selective use of intra-articular injections of corticosteroids. Recent literature has questioned the safety of long term use of NSAIDs and any opiate based medication risks the patient becoming tolerant and dependent on the medication.
Quite often with mechanical pain, mechanical measures are more effective. Therefore, the input of an orthotist is extremely helpful in deciding whether to try corrective or accommodative insoles, braces or callipers or even for bespoke footwear. The benefits of using a walking stick are often overlooked.

Patient positioning is at the discretion of the surgeon and may be governed by the specifics of the case, for instance the need for easy access to the medial aspect of the ankle. When positioning the patient in a supine position, it is recommended that a sandbag is placed under the ipsilateral buttock to aid access to the lateral hind foot. A pack of drapes under the calf lifts the ankle of the operating table and can provide easier access to the posterolateral aspect of the ankle during the procedure. In cases where the surgeon is operating alone, the procedure is straightforward if the surgeon stands and the patient lies in a full lateral position with appropriate supports stabilising the patient.
Fluoroscopy should be available with an image intensifier and a trained radiographer.
A single does of appropriate intravenous antibiotics are administered prophylactically and, in my practise, a thigh tourniquet and exclusion drape are applied. The limb is prepared with Chlorhexidine from toes to tourniquet. In the following case, owing to skin sensitivity, the patient was prepared with alcoholic Betadine.

The patient is in the below the knee back slab for the first two weeks after surgery. At two weeks, the wounds are inspected and re-dressed and a complete, lightweight below-the-knee cast is applied for a further four weeks. Weight bearing is not permitted for the first six weeks after surgery unless transfers are necessary and in my practice, rivaroxaban is prescribed for this duration to prevent thrombo-embolic events. At six weeks, the patient can commence weight bearing in a walker boot which can be removed for sleeping. At twelve weeks, the ankle fusion is assessed radiographically with standing views in two planes before abandoning further immobilisation. There is no need for physiotherapy other than to help patients manage walking aids such as a Zimmer frame. If there is any doubt about the fusion mass on plain radiographic imaging, then further imaging with CT may be helpful.

A new lateral fixed angle locking ankle arthrodesis plate: technique and rate of union. Davies MB, Blundell CM Tech Foot Ankle Surg 2017; 16(4):199-206.
The plate designers assess their experience of more than 80 open ankle fusions using the AnkleFix 4.0 plate for variable degrees of deformity in all planes and determine that their rates of union and other complication rates are comparable with those in the literature. The review covers a heterogenous mix of cases with significant deformity, in revision ankle fusions and dealing with bone loss after total ankle replacement.
Use of a proximal humeral locking plate for complex ankle and hindfoot fusion. Shearman AD, Eleftheriou KI, Patel A et al. J Foot Ankle Surg 2016; 55(3): 612-8.
In a small retrospective study looking at a group of patients with hindfoot fusions including ankle fusion surgery. They audited the concept of a fixed angled locking plate used for ankle arthrodesis and had similar rates of union and complications to Davies & Blundell.
Salvage arthrodesis after ankle replacement. Berkowitz MJ, Sanders RW, Walling AK. Foot Ankle Clin 2012; 4: 725-740.
This is an excellent summary of how to deal with the issue of bone loss in complex hindfoot fusions especially after ankle replacement. The authors suggest a useful algorithm for how to decide when to spare the subtalar joint after a failed total ankle replacement although they use an anterior ankle fusion plate without locked screws.
Revision arthrodesis of the ankle: a 4 cannulated screw compression fixation technique. Tulner S, Klinkenbijl M, Albers G. Acta Orthop 2011; 82(2): 250-2.
Although this paper is primarily written to present a technique, it is a useful paper in reviewing the literature for revision ankle arthrodesis. There are no studies with more than 13 patients with all studies using a multiplicity of techniques with/without bone grafting achieving similar rates of fusion to the Ankle Fix 4.0.
Arthroscopic ankle arthrodesis. Gougoulias NE, Agathangelidis FG, Parsons SW. Foot Ankle Int 2007; 28(6): 695-706.
A retrospective study comparing the outcome of two large groups of patients with either <15 degrees versus >15 degrees of deformity. There was no significant difference between the clinical outcomes or complication rates between the two. However, the lead author’s results may not translate to less experienced surgeons.
Reference
- orthoracle.com











































