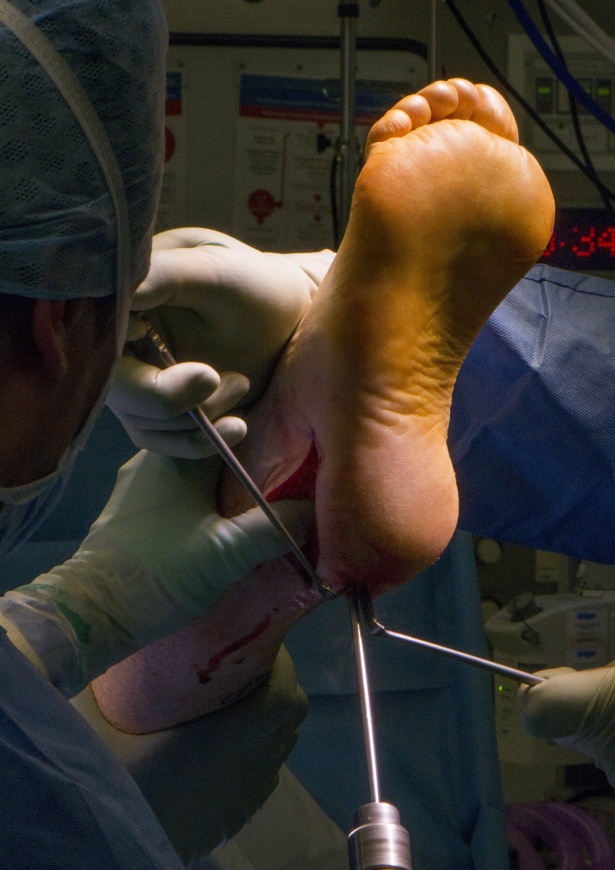
Learn the Correction of the Cavo-varus foot using Orthosolutions Titanium screws and Ultos plate surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Correction of the Cavo-varus foot using Orthosolutions Titanium screws and Ultos plate surgical procedure.
Pes Cavovarus describes a deformity of the foot characterised by a high arch, and a plantar-flexed 1st ray. Whilst some subtle deformities may represent a physiological normal variant, pes cavovarus is often associated with neurological disorders; the commonest being Charcot-Marie-Tooth disease (Hereditary sensori-motor neuropathy).
The deformity progresses as a result of asymmetrical denervation of the flexor and extensor musculature. The power of the Gastocnemius-Soleus, Tibialis posterior and Peroneus Longus muscles are usually preserved relative to the Peroneus brevis, tibialis anterior and intrinsic foot muscles, which are demonstrably weak.
The driver for the deformity is usually a plantar flexion of the 1st metatarsal. In order to engage the ground, the rest of the forefoot compensates by an obligatory supination. The effect of the forefoot supination is (via the forefoot-hindfoot couple) an inversion of the hindfoot, producing the characteristic varus heel. The concept of contracture or tightness of the plantar fascia remains controversial.
In those patients with flexible deformity, joint preserving surgery can be considered and such a case is detailed here treated with osteotomies and tendon transfers.

Pes Cavovarus describes a deformity of the foot characterised by a high arch, and a plantar-flexed 1st ray. Whilst some subtle deformities may represent a physiological normal variant, pes cavovarus is often associated with neurological disorders; the commonest being Charcot-Marie-Tooth disease (Hereditary sensori-motor neuropathy) with a predisposition to progressive weakness and deformity. Progressive unilateral Pes Cavus is unusual, it is associated with spinal compression and spinal tumour and must be investigated.
The deformity progresses as a result of asymmetrical denervation of the flexor and extensor musculature. The power of the Gastocnemius-Soleus, Tibialis posterior and Peroneus Longus muscles are usually preserved relative to the Peroneus brevis, tibialis anterior and intrinsic foot muscles, which are demonstrably weak.
The driver for the deformity is usually a plantar flexion of the 1st metatarsal. In order to engage the ground, the rest of the forefoot compensates by an obligatory supination. The effect of the forefoot supination is (via the forefoot-hindfoot couple) an inversion of the hindfoot, producing the characteristic varus heel. The concept of contracture or tightness of the plantar fascia remains controversial.
Pes Cavovarus deformity may be flexible or stiff, which inevitably has a bearing on management.
Flexibility is assessed clinically, by testing movements and correctability of the ankle, subtalar and Chopart joints, and using the Coleman Block test.
Initial treatment should involve non-operative measures, such as physiotherapy and orthotic management. Corrective Orthotics may be used in flexible deformity, they are designed to compensate for the plantar-flexed 1st metatarsal and correct the obligatory forefoot supination, by incorporating a lateral forefoot build up (posting). In those with uncorrectable deformity, orthotics are less useful as they can only accommodate the deformity.
In those patients with flexible deformity, joint preserving surgery can be considered.
In patients who have non-correctable, stiff deformity, fusion as opposed to joint preserving surgery would be more appropriate.
INDICATIONS:
Joint preserving surgery should be considered in those whose symptoms have not been controlled with non-operative treatment, and in those with severe or rapidly progressive deformity, in order to preserve or improve mobility.
SYMPTOMS & ASSESSMENT:
Patients with Pes Cavovarus have varying degrees of weakness and deformity. Ensure that there is adequate exposure so that feet, ankles, knees, hips, pelvis and trunk alignment can be assessed. Initially examining the patient standing, and walking will provide valuable information regarding the severity of deformity, and degree of functional restriction. When viewed from the front, the arch of the foot will appear high, and the medial aspect of the heel looks prominent (peekaboo sign), there is frequently some degree of clawing of the lesser toes. When viewed from behind, the heel will be varus. The plantar aspect of the foot may reveal callosity or ulceration, frequently under the 1st and 5th metatarsal heads, the base of the 5th metatarsal and the heel.
If the Tibialis Anterior is sufficiently affected, a high stepping foot drop gait may result, and proximal weakness may lead to a trendelenburg gait. The Hindfoot flexibility can be assessed at this stage using a ‘Coleman Block Test’, when the first ray is left unsupported, the block corrects the obligatory forefoot supination, which, in the case of a flexible hindfoot will lead to correction of the heel varus, if the hindfoot is stiff, it will not correct. Flexibility is also assessed clinically, by testing movements and correctability of the calf, the ankle, subtalar and Chopart joints. Each individual muscle group, including quadriceps should be tested and assigned an MRC muscle power grade.
INVESTIGATION:
Antero-posterior and lateral radiographs of the ankle and foot are useful in assessing alignment, deformity and degenerative change, these should be performed weight-bearing.
MRI or CT scans can provide more information on joint and ligament intergrity. MRI spine should be performed in cases of unilateral pes cavus to exclude spinal tumour or compression, and is often used in the investigation of underlying neuropathy.
Nerve conduction studies and electromyography are useful in diagnosing underlying neuropathies and for further assessment of muscle function.
Specialist neurology work-up.
OPERATIVE ALTERNATIVES:
Joint preserving surgery should be considered in flexible deformity, stiff deformity will usually require arthrodesis.
The goal of joint preserving surgery is firstly, to correct the structural deformity in order to re-align the mechanical axis, which is usually achieved with osteotomies and soft tissue release. Secondly to balance the deforming forces using tendon transfers to achieve equipoise.
A dorsal closing wedge osteotomy of the base of the first metatarsal corrects the plantar flexed 1st ray, whilst a Robert Jones procedure (Extensor hallucis longus tendon transfer plus interphalangeal joint fusion of the hallux) is a useful adjunct if there is clawing of the hallucial interphalangeal joint, this is generally insufficient to correct the deformity in the adult. Heel varus is corrected with a lateralising calcaneal osteotomy. An achilles tendon or Strayer procedure is performed if there is a contracture of the achilles or gastrocnemius.
In order to balance the foot, The strong tibialis posterior tendon can be transferred through the interosseous membrane to the outer foot in order to act as an evertor and dorsiflexor of the foot. The strong peroneus longus may be tenodesed to the relatively weak peroneus brevis.

Pes Cavus correction is usually performed under a general or spinal anaesthetic.
A popliteal regional block is performed pre-operatively.
Prophylactic antibiotics are administered intra-venously.
A thigh tourniquet is inflated immediately prior to skin preparation and after a WHO check.
The patient is positioned supine on the table, a sandbag is placed under the ipsilateral buttock which rotates the leg inwards, allowing good access to the lateral heel. The extended lateral approach exploits the watershed between the posterior peroneal, the posterior tibial and the lateral plantar angiosomes, preserving the vascularity and reducing ischaemia to the lateral skin flap. The incision is posterior to the sural nerve reducing injury and neuroma formation.

A below knee Backslab is applied in the operating room.
The leg is elevated.
The leg is immobilised in a below knee plaster for 6 weeks, non-weight bearing, during which time daily low molecular weight heparin is administered.
At 6 weeks radiographs are performed to ensure union across the osteotomy sites has occurred.
From 6-12 weeks full weight bearing in a pneumatic boot is encouraged, during which time the boot can be removed to allow gentle exercise, and physiotherapy should commence, concentrating on maintaining flexibility and isolating and gentle strengthening of the tibialis posterior tendon. Excessive load, inversion and plantar flexion should be strictly avoided

Foot Ankle Surg. 2010 Sep, Flexible cavovarus feet in Charcot-Marie-Tooth disease treated with first ray proximal dorsiflexion osteotomy combined with soft tissue surgery: a short-term to mid-term outcome study.
Leeuwesteijn, de Visser, Louweren.
Retrospective study 33 patients with dorsiflexion osteotomy of 1st ray with associated tendon transfers and calcaneal osteotomies. Good results in 90% short to mid term.
Foot Ankle Clin Sep 2001
Combined calcaneal and metatarsal osteotomies for the treatment of cavus foot.
Sammarco, describes combined metatarsal and calcaneal osteotomies to reduce arch height, increase ankle stability and reduce pain.
Foot Ankle Int Oct 2018
Comparison of hindfoot osteotomies in the correction for varus hindfoot correction.
Closing wedge in combination with closing wedge osteotomy achieved greatest correction when compared to lateralising or Dwyer closing wedge osteotomy alone.
Pfeffer. G
Foot Ankle Clin 2013
joint sparing correction of cavovarus feet in Charcot Marie Tooth disease: What are the limits?
Emphasises the range of deformities and weakness in Charcot Marie Tooth disease, and the need for an individualised approach to surgery.
Winson.I
Reference
- orthoracle.com


























































