Learn the Cubital tunnel decompression: In-situ distal to proximal release of the ulnar nerve surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Cubital tunnel decompression: In-situ distal to proximal release of the ulnar nerve surgical procedure.
Ulnar nerve compression most commonly occurs where the nerve passes behind the medial epicondyle at the elbow, passing through the cubital tunnel and in between the two heads of the flexor carpi ulnaris muscle (FCU) to enter the forearm. The nerve becomes compressed due to a combination of it being pulled against the bone when the elbow is flexed, and being squashed from its superficial side by the fascia, ligaments and fibrous bands that form a roof above the cubital tunnel along with arcades of blood vessels. Muscles that cross over the ulnar nerve can also compress it, such as the triceps (at the arcade of Struthers), FCU, and, when present, anconeus epitrochlearis (a muscle that passes from the medial epicondyle to the olecranon, found as part of the roof of the cubital tunnel in approximately 1 in 7 people- do not confuse this with the much bigger anconeus muscle, found on the lateral aspect of the elbow).
Symptoms from ulnar nerve compression may be felt in the ulnar side of the hand, the medial aspect of the elbow, or along the ulnar side of the forearm; holding the elbow flexed and in particular leaning on the inner aspect of a flexed elbow will bring on symptoms (which are often felt at night, when many people flex their elbows).
Unless the nerve is unstable (moves across the medial epidondyle to the front of the elbow with flexion above 90 degrees), decompression of the nerve where it lies by division of the structures that lie superficial to the nerve and compromise it will usually improve intermittent symptoms and prevent deterioration of permanent nerve loss in the hand and forearm (sensory loss in the little and ring fingers, atrophy of the intrinsic muscles of the hand with impairment of thumb grips and fine motor skills).
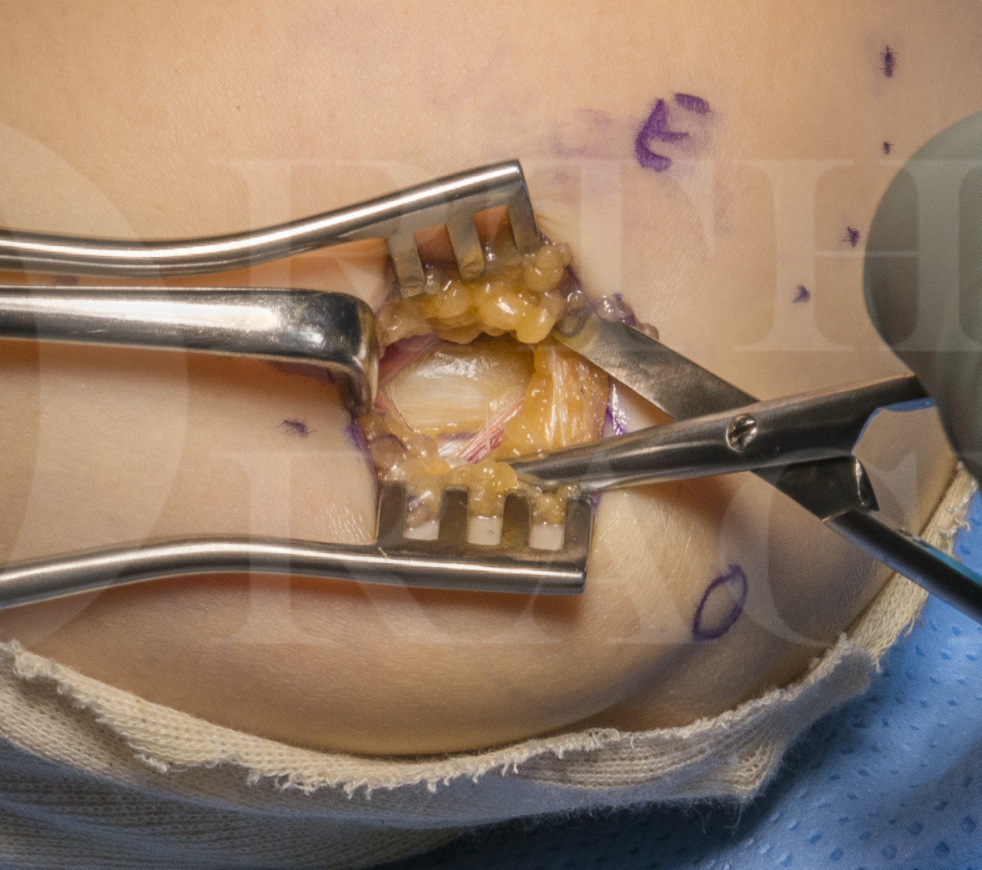
Most surgeons are trained to identify the nerve proximal to the elbow and trace its path down into the forearm, which involves an incision that extends both above and below the elbow; particularly in patients with fat arms, identifying the nerve proximal to the cubital tunnel can be surprisingly difficult! The nerve can be found reliably where it passes between the two heads of FCU and if the nerve is identified at this site, the proximal dissection and release can be safely and easily preformed without extending the skin incision proximal to the medial epicondyle, so minimising the risk of damage to the medial cutaneous forearm nerve branches that pass close to the medial epicondyle.
Endoscopic techniques have been described for cubital tunnel release, but these require specialist equipment and offer limited practical advantages over open techniques of cubital tunnel decompression other than utilising smaller incisions. With practice, surgeons can reduce the length of skin incision used for open decompressions as they and their surgical teams become familiar with the surgical anatomy and optimal positioning of retractors.
Dominic Power has described his technique for cubital tunnel decompression on Orthoracle, the indications for which and technique are similar in many respects to the procedure described here; important differences include the positioning of the arm to make the role of the first surgical assistant easier, the site and extent of the incision to avoid potential damage to cutaneous nerves, and the technique for proximal release.
Surgeons should be aware of the uncommon but encountered potential for compression of the ulnar nerve at the wrist where the ulnar nerve passes through Guyon’s canal. Tahseen Chaudhry has described his technique for a single incision combined carpal tunnel and Guyon’s canal release on Orthoracle and readers will also find of interest Dominic Powers revision technique:
Revision cubital tunnel release with submuscular transposition and application of Axoguard

INDICATIONS
Intermittent ulnar nerve symptoms that do not respond to provocation avoidance.
Permanent sensory or motor loss in an ulnar nerve distribution with neurophysiological confirmation of pressure on the ulnar nerve at the elbow.
SYMPTOMS & EXAMINATION
Symptoms:
Pain, tingling or numbness in the ulnar side of the hand (invariably the little finger; often ring, sometimes middle fingers
Pain in the medial aspect of the elbow.
The above radiating along the ulnar side of the forearm.
Symptoms provoked by holding the elbow flexed and in particular leaning on the inner aspect of a flexed elbow.
Night waking with the above symptoms.
Numbness as above first thing in the morning.
Symptoms improved by straightening elbow.
Examination findings:
Sensory
Altered fine touch sensation in an ulnar nerve distribution (usually little and ulnar ring, although may involve middle; note that patients often don’t have an anatomically-characteristic watershed along the midline of a digit).
Dorso-ulnar hand (although often less involved than digits in practice)
Assess objectively
Static 2-point discrimination (innervation density)
Semmes-Weinstein monofilament testing (sensory threshold)
Much more pragmatically, the Tens Test (Strauch et al (1997) Plastic and Reconstructive Surgery 99:1074-1078)
Motor
Intrinsic muscles of hand
Adductor Pollicis (Ad Pol)- Froment’s sign (well explained in Cubital Tunnel Indications section)
1st dorsal interosseous (1stDIO)- combined 1stDIO and AdPol wasting causes the visible and palpable wasting of the muscles of the 1st web space (thumb to index finger)
Interossei- guttering on the dorsum between the metacarpals
Hypothenar eminence
Extrinsic muscles
Flexor digitorum profundus (FDP) to little, ring +/- middle fingers
IMAGING
ALTERNATIVE OPERATIVE TREATMENT
Different surgical procedures are used, including
Endoscopic decompression
Open in-situ decompression proximal-to-distal
Anterior ulnar nerve transposition
sub-cutaneous
sub-muscular
Medial epicondylectomy
NON-OPERATIVE MANAGEMENT
Provocation avoidance
not holding the elbow bent for long periods
not leaning on the inner aspect of the elbow and proximal forearm
adapting desk spaces to prevent flexion and pressure
splinting the elbow straight when sleeping
Nerve gliding exercises
Attention to shoulder and scapular posture to prevent compromise at the thoracic outlet (the “double-crush phenomenon”)
CONTRAINDICATIONS
Presence of a clear reason to transpose the nerve
Ulnar nerve instability (either before or on completion of in-situ decompression)
Unhealthy cubital tunnel bed (e.g., osteophyte, synovial or ganglion encroachment)
Significant cubitus valgus
Medical contraindications to general or regional anaesthesia (consider local anaesthetic with adrenaline if symptoms justify the surgical risks)

Surgery is usually performed supine with the arm supported upon an arm table, although if local anaesthesia is used, the patient may be more comfortable lying supine without an arm table but with their hand resting on the operation table beside their head, from where the arm can be moved intraoperatively to optimise surgical lines of sight or for comfort. Some surgeons prefer their patients to lie prone, particularly if the patient has a stiff and/or painful shoulder, although this position makes support for the hand and arm more difficult to achieve. Local anaesthetic surgery can be undertaken without a tourniquet if adrenaline is used.

Aside from the usual observations during the recovery period following a musculoskeletal procedure performed under general anaesthetic, very few specific steps need to be taken prior to discharge. The ulnar nerve will often be blocked by the infiltration of local anaesthetic, so do not be surprised if there is altered sensation in an ulnar nerve distribution. Active elbow mobilisation should be encouraged within limits of comfort straight away, and the bulky dressing should be removed after 2-3 days, leaving the adhesive dressing intact. I recommend that scooping and lifting should be avoided for 4-6 weeks due to the potential for discomfort from the separated heads of FCU, but as no muscle repairs have been needed, there are no restrictions to activities other than to be pain-limited. Most patients only require regular oral analgesics for up to a few days, thereafter using them as required. The presence of throbbing or marked pain (i.e., pain not controlled by oral non-opioid analgesics and topical ice) should raise concern about potential complications (such as haematoma formation, un-recognised nerve injury, or early infection or complex regional pain syndrome) and so should prompt urgent clinical review.
Despite using absorbable sutures, I prefer the intra-dermal suture to be removed after 2-3 week where possible to avoid inflammatory spots arising where the suture enters and leaves the skin.
Unless there was permanent pre-operative neurological loss, most patients can be discharged once their pre-operative symptoms can be confirmed to be improved, which is usually after the first post-operative review at 2-3 weeks.
Pain or neurological deterioration that persists for more than 6 weeks after surgery should prompt consideration of investigation; pain suggestive of haematoma formation or nerve instability is best assessed with an ultrasound, and persisting neurological deterioration with nerve conduction studies. Treatments that may be appropriate would be determined by the investigation results and the clinical course of the patient.

Simple decompression or subcutaneous anterior transposition of the ulnar nerve for cubital tunnel syndrome
Nabhan et al (2005)
Journal of Hand Surgery (British and European Volume) 30B: 5: 521-524
A randomised study comparing in-situ decompression against anterior sub-cutaneous transposition for neurophysiologically-confirmed ulnar nerve compression in the cubital tunnel, showing no statistically significant clinical outcome difference between the two technique groups, and no statistical difference in the degree of improvement in the neurophysiological investigations between the two techniques over the 9 month follow-up period. This paper confirms that in-situ decompression is a valid technique to use for primary ulnar nerve decompression surgery.
Treatment for ulnar neuropathy at the elbow
Caliandro et al (2016)
Cochrane Database of Systematic Reviews https://doi.org/10.1002/14651858.CD006839.pub4
A systematic review of 4 randomised studies comparing in-situ decompression against anterior transposition ( sub-cutaneous or sub-muscular) for ulnar nerve compression in the cubital tunnel, showing no statistically significant clinical outcome difference between the in-situ decompression and anterior transposition in the 3 included studies, and no difference in the degree of improvement in neurophysiological investigations between the two techniques in the 2 included papers. The rate of deep infection and superficial infection was greater in the transposition groups. This systematic review found that there is moderate-quality evidence that in-situ decompression is equally effective when compared to anterior transposition for idiopathic ulnar nerve compression with a lower risk of infection.
Patient-reported outcomes after in-situ cubital tunnel decompression: a report in 77 patients
Yeoman et al (2020)
Journal of Hand Surgery (British and European Volume) 45B: 1: 51-55
Prospective cohort study of QuickDASH-reported outcome of in-situ decompression at a mean of 17 months showing significant improvements in patient-reported scores, the degree of improvement correlating with patient satisfaction, and finding lower levels of satisfaction in patients with pre-operative weakness.The study confirms improvements with in-situ decompression, and that intervention before the onset of permanent motor loss if important.
Reference
- orthoracle.com



































