Learn the Diagnostic Wrist Arthroscopy (using Acumed ARC Tower ) surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Diagnostic Wrist Arthroscopy (using Acumed ARC Tower ) surgical procedure.
This is a detailed step by step instruction through the set up and procedure of a diagnostic wrist arthroscopy using the Acumed TM ARC Tower traction system.
Wrist arthroscopy is an expanding speciality and with the improvement in diagnostics with 3T MRI scanning it is being used less for diagnostic procedures and more for definitive surgical interventions.
Diagnostic wrist arthroscopy is an excellent way to become familiar with the procedure and develop skills to advance onto more invasive procedures using wrist arthroscopy.
If a diagnostic arthroscopy is used to confirm a MRI or clinical finding then an further open or arthroscopic procedure can be often performed at the same sitting if the patient has been appropriately consented.
Despite the improvement in MRI scanning and interpretation, wrist arthroscopy is still the gold standard for many conditions although the invasive nature and cost of the procedure certainly has some disadvantages compared with MRI. Conditions particularly difficult to determine on MRI are Luno-triquetral interosseous ligament (LTIL) injuries and injuries causing symptomatic mid-carpal instability. Bony injuries are much better seen on MRI and unlikely to be missed due to the oedema seen in the bone.
Following a diagnostic wrist arthroscopy, patients are usually placed in plaster cast for 1 week for comfort then allowed to mobilise to reduced stiffness. The individual post-operative rehabilitation or further intervention will clearly depend on the arthroscopic findings and patient wishes.
Complications in diagnostic wrist arthroscopy or rare and usually minor however it has been shown that when surgeons are learning this skill, tendon injuries and iatrogenic cartilage injuries are more frequent.

Indications
A diagnostic wrist arthroscopy is performed to confirm a clinical or radiological finding and to plan further interventions. These further interventions may be immediate arthroscopic or open surgery, a period of immobilisation or physiotherapy with or without splinting.
Wrist arthroscopy is the gold standard for assessing specific intra-articular abnormalities such as cartilage damage (to diagnose a pain source or plan salvage surgery such as limited wrist fusions), ligament injuries (particularly interosseous carpal ligaments – scapholunate and luno-triquetral) TFCC (triangular fibrocartilage complex) injuries, intra-articular loose bodies or ganglia, synovitis and adhesions.
Wrist arthroscopy is also useful to exclude these abnormalities in cases of mid-carpal instability where the pathology may be ligament laxity and muscle weakness rather than ligament rupture.
Wrist arthroscopy can also be used as an adjunct to other surgical procedures (arthroscopic assisted) such as intra-articular distal radius or scaphoid fracture fixations to check reduction during and after fixation.
Wrist arthroscopy can also be used beyond the diagnostic procedure in interosseous ligament repairs or reconstructions, limited wrist fusions (STT – scapho-trapezoid-trapezium, 4CF – four corner fusion), capsular shrinkage (for midcarpal instability or lax ligaments), bony resection (radial styloidectomy, distal scaphoid excision, proximal hamate excision, Wafer procedure of the ulna), TFCC repairs or reconstructions, joint debridement (synovectomy, arthrolysis or joint washout), DRUJ (distal radioulnar joint) debridement and assessment and ganglia excision.
Symptoms
The symptoms experienced will depend on the underlying pathology however in the main the operation is undertaken for pain or dysfunction. In acute settings it is usually performed to diagnose ligament tear and in the more chronic setting the pathologies mentioned in the indications section.
Examination
Examination to proceed a diagnostic wrist arthroscopy will be a focused wrist examination.
If there are clinical concerns about limitation or pain during pronation and supination the proximal radio-ulna joint must also be examined.
The contra-lateral wrist is examined initially for two reasons. One to discover what is normal for the patient as laxity, clicks and clunks can be normal if asymptomatic. Secondly as some of the examination tests stress the wrist in unusual ways, the patient is then aware what to expect and what is normal (some tests such as Lichtman mid-carpal shift test can be uncomfortable or a ‘strange feeling’ on a normal wrist – especially if there is a positive finding).
The problematic joint is assessed for swelling, deformity and previous scars on inspection.
It is then palpated systematically usually starting away from the most painful site and progressing around the wrist generally over the radio-carpal, mid-carpal and distal radio-ulna joint lines but also more specifically over bony prominences such as the scaphoid tubercle, pisiform and hook of hamate. Palpation may also yield more information with different wrist positioning i.e. in flexion more of the scapho-lunate ligament is exposed to palpation and in ulnar deviation more of the waist of the scaphoid is palpable beyond the radial styloid. On the ulna side of the wrist tenderness over the Extensor carpi ulnaris (ECU) may actually be deeper pain within the TFCC and can be differentiated by palpation in supination where the tendon lies more dorsally and pronation where it lies more ulnarly.
Following palpation the range of movement is assessed – flexion (75), extension (70), supination (85), pronation (70) and radial (20) and ulnar deviation (35) – normal ranges in degree provided in brackets.
Special tests then can be performed based on clinical suspicion-
Kirk-Waston test for scapholunate instability (also promotes pain but no clunk in STT arthritis)
Kleinman shear test and Reagan test for Luno-triquetral instability
Lichtman midcarpal shift test for midcarpal instability.
Pisiform pressure to elicit symptom improvement for mid-carpal instability
DRUJ squeeze in supination and pronation promotes pain in DRUJ arthritis/synovitis
DRUJ stability testing for TFCC tear (including Piano key test)
Ulna impaction or grind tests for TFCC injuries and synovitis
Piso-triquetral shearing for arthritis
Ice-cream scoop movement to test for ECU pain/subluxation
It may be difficult to elicit a positive result in some of these tests especially in the acute settign if pain is a major issue and the patient’s wrist is not relaxed during the examination.
Investigations
Investigations include plain PA and lateral radiographs of the wrist with the addition of a clenched fist view if a scapholunate ligament rupture is suspected.
On these radiograph we are looking for arthritis, fractures, ligament injuries (identified with increase interosseous gaps on the PA and clenched fist views and scapho-lunate and capito-lunate angles on the lateral view).
An MRI scan (preferable 3T) is the next investigation for many patients as this can identify occult fractures and ligament injuries and other soft tissue abnormalities such as synovitis and ganglia.
If an MRI in contra-indicated due to patient co-morbidities or claustrophobia then a CT scan or SPECT scan (single-photon emission computed tomography) is useful for identifying pathology.
Non-operative Management
Non-operative management will depend completely on the pathology and symptoms.
Diagnostic wrist arthroscopy is used in acute conditions for a diagnosis after trauma or in chronic conditions with continue pain or instability.
For acute patients analgesia and splinting usually precede the arthroscopy. For chronic patients depending on the problem then analgesia, splinting, activity modification, physiotherapy with wrist strengthening or a steroid joint injection may be useful in symptom control.
For mid-carpal instability patients, a wrist splint which applies Pisiform pressure to support the ulnar carpus can also be useful.
Alternative operative Management
For diagnostic arthroscopy there is no surgical alternative.
Contraindications
The only contra-indications to wrist arthroscopy are a patient who is not fit enough for the procedure, a wrist which it is not possible or extremely difficult to scope due to tightness or stiffness (major surgery previously or inexperience of surgeon), anti-coagulation therapy which is unsafe to stop and ongoing chronic regional pain syndrome (CRPS).

Pre-operative preparations and Equipment
The operation can be performed under general (GA) or regional anaesthetic.
As many procedures are undertake for possible ligament injury it is essential to perform an examination under anaesthetic (EUA) then an EUA with fluoroscopy to gain as much information as possible to aid diagnosis. The clinical examination in the outpatients department, the EUA and the operative findings are then all combined to assess what findings are clinically relevant.
NB – Only surgically treat findings which correlate with clinical findings e.g. If a patient presents with pure radial sided wrist pain and an arthroscopy finds only a TFCC tear – DO NOT TREAT – as this is not symptomatic.
A single dose of antibiotics are given pre-operatively and no thromboprophylaxis is used unless the patient is under a GA.
With experience, the duration of a diagnostic wrist arthroscopy is around 15mins however if a second procedure is going to follow the diagnosis then the duration of surgery may be much longer. Patients under axillary block often notice tourniquet discomfort between 90-120 minutes (this can be prolonged with use of local infiltration beneath the tourniquet and/or distraction techniques such as watching a film or listening to music on a portable device).
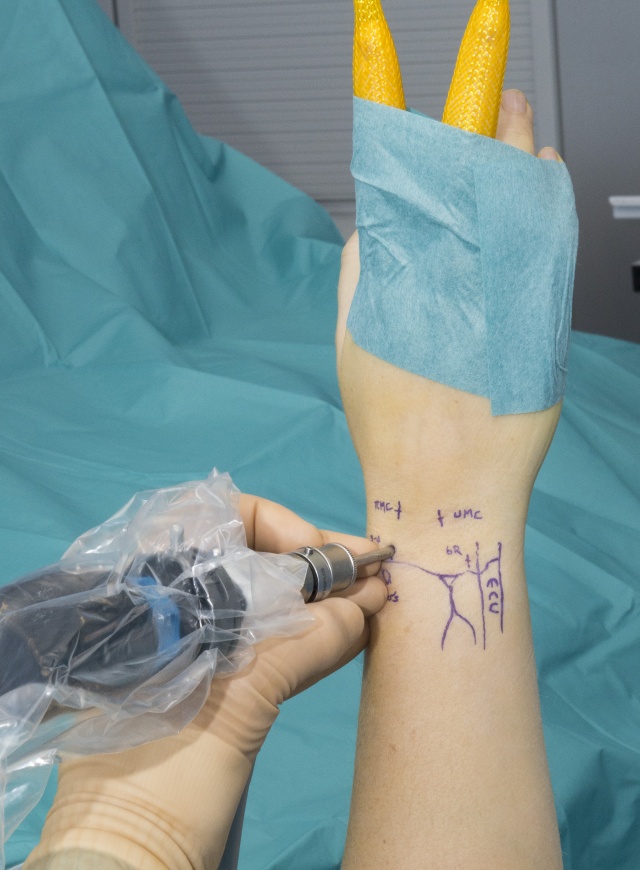
The patient is lay supine with an arm on the arm board, the arm prepped and draped, a sterile tourniquet applied, the hand held in traction and the skin markings completed PRIOR to exsanguination with a sterile Esmarch..
Kit
Arthroscopy tower or gantry, finger traps, sterile tourniquet, sterile Esmarch, OlympusTM arthroscope 30 degree (1.9, 2.4 or 2.7mm), shaver, ablator, white needle 16 gauge, adhesive tape (around base of finger traps), straight artery clip, 11 blade for knife, wrist arthroscopy probe, saline in 50ml syringe and connector to attach to arthroscopy trochar.

The post operative plan for patients undergoing a diagnostic wrist arthroscopy will vary greatly depending on the diagnosis discovered and treatment plan.
In the initial post operative phase the patient is in a plaster cast for 1 week and then the wounds are reviewed and physiotherapy can begin to mobilise the patient. A splint may be provided for comfort and then the specific regimen related to diagnosis or plan for a subsequent surgery can be carried out.
Complications –
Iatrogenic cartilage damage, tendon injury, nerve injury (PIN – 4-5 RC portal, dorsal sensory ulnar branch – 6U portal), infection, CRPS, failure of diagnosis or procedure if the wrist is very scarred or tight and post operative stiffness.
Rates of complication can be seen in the Results section literature.

Leclercq C1, Mathoulin C1; Members of EWAS.
Complications of Wrist Arthroscopy: A multicenter study based on 10,107 arthroscopies.
J Wrist Surg. 2016 Nov;5(4):320-326. Epub 2016 May 17.
In summary the data was collected using questionnaires from 36 centres. They noted a 6% complication rate. 5% serious 1% minor. This included a failure to achieve procedure 1.16%, nerve lesion 1.17%, iatrogenic cartilage lesion 0.5%, CRPS 0.5%. Wrist stiffness, hematomas and tendon injury were less common. Those surgeons performing less than 25 arthroscopies a year were seen to have a significant increased complication rate.
Complications of wrist arthroscopy
Arthroscopy. 2012 Jun;28(6):855-9. doi: 10.1016/j.arthro.2012.01.008. Epub 2012 Apr 6.
Leclercq C1, Mathoulin C1; Members of EWAS.
Complications of Wrist Arthroscopy: A multicenter study based on 10,107 arthroscopies.
J Wrist Surg. 2016 Nov;5(4):320-326. Epub 2016 May 17.
In summary the data was collected using questionnaires from 36 centres. They noted a 6% complication rate. 5% serious 1% minor. This included a failure to achieve procedure 1.16%, nerve lesion 1.17%, iatrogenic cartilage lesion 0.5%, CRPS 0.5%. Wrist stiffness, hematomas and tendon injury were less common. Those surgeons performing less than 25 arthroscopies a year were seen to have a significant increased complication rate.
These cases were not all diagnostic scopes and more complex procedures were performed in many cases.
Free link to paper https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5074840/
Ahsan ZS1, Yao J.
In summary this was a systematic review of 11 papers 1994-2010. A complication rate of 4.7% was seen. Complications included nerve injury, tendon injury and infection.
Reference
- orthoracle.com















































