Learn the Dupuytrens contracture: Collagenase (Xiapex) injection and manipulation surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Dupuytrens contracture: Collagenase (Xiapex) injection and manipulation surgical procedure.
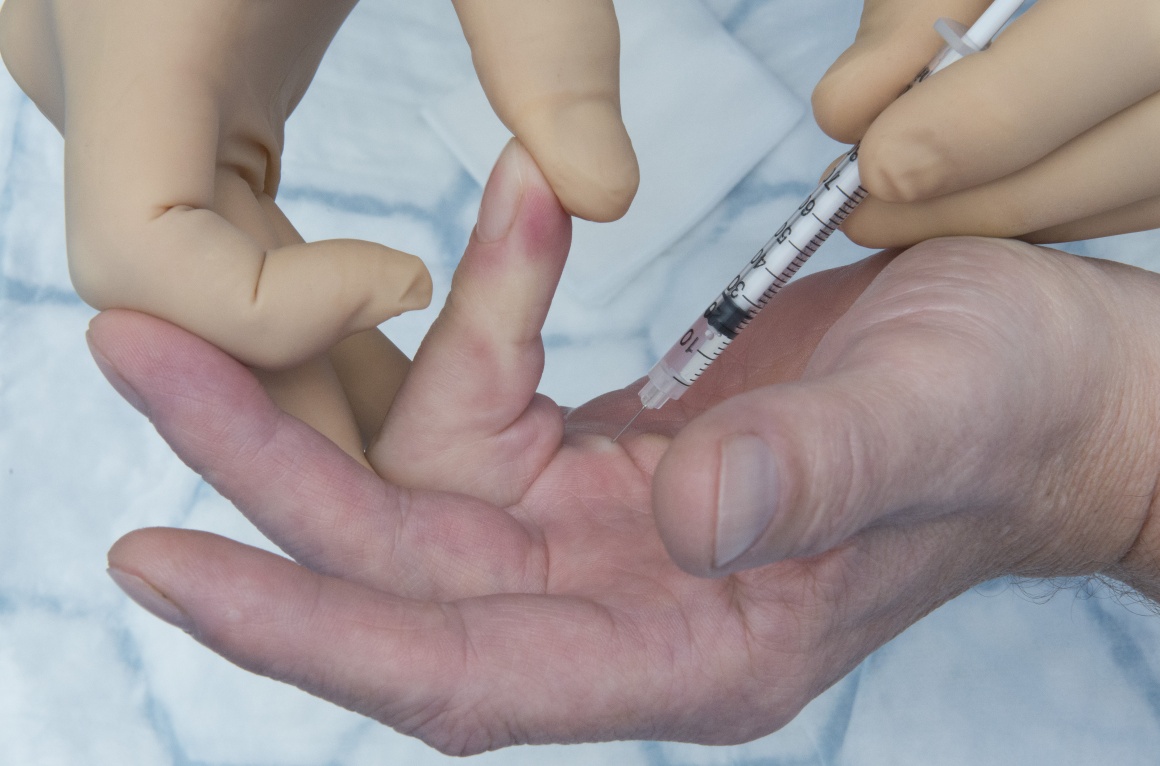
This is a detailed step by step instruction through an injection of a pretendinous Dupuytren’s cord with collagenase enzyme.
Dupuytren’s contracture is a relatively common condition which causes a histological alteration in a number of fascial structures within the palmar surface of the hand. It is a clinical diagnosis and only rarely when there is a single nodule which has not caused any contracture in the early stages can it be difficult to diagnose. 75% of cases occur in the ulna 2 digits.
There is no current cure for the disease however there are 4 main groups of treatment options to improve contractures. These options are needle fasciotomy, fasciectomy, dermo-fasciectomy and collagenase injections. Within the fasciectomy group terminology becomes confusing with many terms being used synonymously despite original descriptions differing. Examples are focal, segmental and limited fasciectomy. There is also variation in a dermo-fasciectomy with a small fire-break skin grafts or a larger graft covering a clear anatomical section e.g. volar finger between MCPJ and PIPJ creases.
In addition, adjuncts to surgery such as temporary external fixators or salvage options such as amputation are also included in the Dupuytren’s treatment armamentarium.
Collagenase clostridium hostolyticum (XiapexTM in the UK, XiaflexTM in the USA) injections have be used for Dupuytren’s contracture since FDA (food and drug administrations) approval in 2010. Collagenase is an enzyme which breaks down the peptide bonds in the collagen within Dupuytren’s tissue. AUX-I and AUX-II collagenase break the bonds within Type 1 and Type 3 collagen.
The injection is performed either in a clinic or theatre setting without any anaesthetic and then 1-3 days later (by the distributers recommendations). The finger is manipulated under local anaesthetic (LA) and then a review by the hand therapists and a thermoplastic night splint is applied for 3 months.
In July 2017 NICE (National institute for health and care excellence) in the UK produced guidance for use of collagenase in the NHS. This recommended that a palpable cord could be treated if there is moderate disease (MCPJ contracture 30-60 degrees and PIPJ less than 30 degrees) and one injection per treatment session.
A multicentre RCT the DISC trial (Dupuytren’s interventions surgery versus collagenase) began recruiting in the UK in May 2017 and will have a 2 year follow up for fasciectomy versus collagenase completed by October 2021.
Complications include failure of complete correction (common with severe PIPJ disease where the joint capsule and ligaments are contracted), recurrence (very common over time with rates of around 50% at 5 years depending on disease severity, joint involved and amount of correction achieved at manipulation), tendon rupture, neurovascular injury (rare and usually neuropraxia), skin tear during manipulation, pain and swelling post injection, infection, stiffness and allergy to collagenase.

Pathology and Anatomy
Dupuytren’s disease is an inherited autosomal dominant trait with variable penetrance and expressivity. Normal fascia is composed mainly of type I collagen. In Dupuytren’s there is a increase of type III collagen (as also seen in wound healing) and myofibroblasts which are a contractile cell derivative from the fibroblast.
With this contractile potential the normal anatomical ‘Bands’ within the hand can become contracted ‘Cords’.
In addition to ‘Cords’, ‘Nodules’ are seen when a bulk of Dupuytren’s tissue appears in one site and ‘Pits’ are seen when the skin fibres contract and pull small areas of skin down towards the deeper cords in the palm.
Examples of the anatomy will be shown in the surgical pictures however as an overview the bands/cords are:
Pretendinous (band/cord) – a continuation of the palmaris longus and palmar fascia which is in line with each digit and inserts around the flexor sheath at the level of the MCPJ crease (a central cord can continue in this line along the flexor sheath to the DIPJ).
Natatory (ligament/cord) – transverse cords which span between the web spaces blending with the pretendinous band/cord and spiral band/cord
Spiral (band/cord) – longitudinal structure superficial to neurovascular bundle (NVB) crossing from pretendinous band/cord to blend with lateral digital fascia, when contracted this pulls the lateral digital fascia/cord centrally and as the NVB is enclosed by Grayson’s and Cleland’s ligaments which are attached to the lateral digital fascia the NVB is then pully more centrally in the finger at the level of the MCPJ crease.
Lateral digital (fascia/cord) – longitudinal structure close to the skin running almost up the lateral midlines of the fingers attached to Grayson’s and Cleland’s ligaments.
Retrodigital (fascia/cord) – distal continuation of lateral digital fascia/cord which may cause DIPJ contracture.
Commisural (band/cord) – similar to Natatory but of the 1st web space
Legueu and Juvara (septa/cord) – vertical structures which separate the distal palm into sections with NVB and lumbrical then flexor sheaths in alternating sections.
Grapow (fibre/cords) – small vertical structures which tether the palmar skin to the deeper fascia and provide stability of the skin and cause pitting when contracted.
Indications
Dupuytren’s contracture affect around 2 million people in the UK.
A patient will present for treatment usually for 3 reasons.
They have lumps in the palm and are unsure of the diagnosis and may be worried about a diagnosis or cancer. – These patients can be reassured based on a clinical diagnosis, educated on the condition and discharged.
They are aware of the diagnosis and the tightness of the palm or nodules are a nuisance but no clear fixed flexion deformity – these patients are best educated about the condition and the likely recurrence rates and therefore avoidance of very early surgery to avoid scarring and increased future complications of repeat surgery. If they still would like intervention in specific cases (e.g. professional pianist who’s span is reduced or tree surgeon with large nodules but no contracture making gripping difficult and climbing unsafe – reasonable surgical indications) they have two options in the UK. One is to have treatment in the private sector and the other is for the surgeon to apply for specific funding on individual grounds for the treatment to the funding body.
The patient has a contracture of the digit causing dysfunction. In the UK patients can undergo funded treatment for Dupuytren’s contractures based of certain guidelines (often falling under ‘Procedures of limited clinical value’). In the authors region this states if there is a progressive PIPJ contracture or an MCPJ contracture of 30 degrees or more then treatment can proceed. These value are often the point at which dysfunction is increasing due to the contracture.
Symptoms
Dupuytren’s disease is a non-painful condition. Although the condition can be itchy or sore when active proliferation is taking place, or painful when gripping if a large nodules are compressed, if pain is a main feature of the presentation then a rare but serious diagnosis of fibrosarcoma should be excluded.
Dupuytren’s contracture is a spectrum of severity and can range from a mild inconvenience to a disabling condition with all ten digits severely affected.
Patients complains of aching or cramping in the hands, a feeling of tightness and the inconvenience of the contracted digit of poking then in the eye when washing their face, catching on their clothes when trying to get money out of their pocket and sticking on door handle after they have opened them.
Dupuytren’s Diathisis is a collections of signs and conditions which are seen to suggest a worse prognosis in terms of disease progression and recurrence. This is made up of age <50, male, bilateral disease, radial sided disease (thumb/index finger), family history and ectopic disease. Ectopic sites include the dorsal PIPJ nodules (Garrod’s pads), penile fibrosis (Peyronie’s disease), plantar fibrosis (Lederhose’s disease).
Examination
Inspection usually reveals cords, nodules and pits within the palms and fingers.
It should be noted from the history which specific fingers are troubling the patient especially in more severe disease when all fingers are affected and multiple treatments and recurrences have already occurred.
Joint contracture angles should be measured and recorded and it is useful to isolate each joint and record the combined and individual joint contractures. This is performed with a small finger goniometer on the dorsum of the finger. Initially the whole finger is extended maximally and the joint angles recorded. Following this the MCPJ is fully flexed and PIPJ maximal extension is recorded then the PIPJ is maximally flexed and the MCPJ extension angle recorded.
This differential will help the surgeon identify if there is a spanning cord contracting both joints and help with prognosis to predict the post-operative correction.
As a general rule all MCPJ contractures caused by Dupuytren’s no matter how severe will be corrected by treatment. Any PIPJ contracture above 60 degrees is likely to remain with some contracture post treatment. This is due to the collateral ligament and volar plate contractures which can be released intra-operatively to provide a greater extension but at greater risk of joint stiffness, and loss of flexion.
After previous surgery a digital Allen’s test and assessment of sensation are also useful to record if further intervention is being planned.
Further examination of ectopic sites can be undertaken if necessary although usually only the dorsal PIPJ disease of Garrod’s pads is reviewed.
Investigations
There are no formal investigations for Dupuytren’s disease unless there is a concern regarding pain and a possible diagnosis of sarcoma. In this case a USS or MRI may be performed. This may also be necessary in an isolated nodule where diagnosis is unclear.
Non-operative Management
The best non-operative treatment is patient education and reassurance which includes advice on the stage of disease progression which treatment is advised.
Non-operative management with splinting or physiotherapy have not shown to be affective. Radiotherapy is one option used to prevent disease progression however the evidence on its effectiveness is limited. The author does not use this in their treatment pathway.
Alternative operative Management
As discussed the alternative treatment options to Collagenase injection include – needle fasciotomy (aponeurosis), fasciectomy, dermo-fasciectomy, amputation and an adjunct of temporary external fixation or joint arthodesis.
Contraindications
Collagenase is contra-indicated where a clear cord cannot be identified to inject, in pregnancy, breast feeding and in patients who have received Tetracycline antibiotics within the last 14 days.
Anti-coagulation treatment must be taken into account however is not an absolute contra-indication.
Further research is now published to safely allow two vials of collagenase in one treatment session however if a patient opted to treat all 4 fingers on one hand treated in one sitting or is keen to remove all the lumps in their hand (e.g. to wear a wedding ring again) the this is not possible with collagenase injection alone.
Previous surgery or skin graft or collagenase injection is not a contra-indication.

Pre-operative preparations and Equipment
The injection may be performed in the clinic or theatre setting.
The vials of collagenase are reconstituted as required (detailed in operative technique).
The hand is laid on a clean drape. No further equipment is required.
No antibiotics or are thromboprophylaxis required.
Patients are warned about the likely affects over the following 48 hours of local bruising or swelling which can be very marked in some individuals and lymph node pain in the medial elbow and axilla.
They are also warned that, especially with MCPJ contractures, they may snap the cord themselves if they catch the finger or when getting out of bed in the morning – this is not a problem, however they are still recommended to attend the manipulation to achieve the maximal correction possible.
A simple dressing is used post operatively.

Following the injection the patient is kept in the department for 1 hour (30 mins in manufacturers guidelines) for observation of any adverse effects. During this time their observations of pulse rate, oxygen saturation and blood pressure are recorded twice.
The patient reattends at 1-3 (or 1-7) days post injection for the manipulation and following manipulation and splintage and any wound care needed the patient is seen biweekly if they have a large skin tear until it is healed or at 3 months if all is well.
At this point they are discharged if no further intervention is required.
If patient are struggling with stiffness or have other queries the hand therapist will refer them back for review earlier if concerned.

As noted all MCPJ contractures are expected to regain full range of movement. The more severe the PIPJ contracture the less likely a full correction will be achieved. In addition the prolonged flexion of the PIPJ appears to attenuate the central slip slightly and despite a very good correction there may be a lag due to the extensor function which it is hoped will resolve with night splinting.
Dupuytren Contracture Recurrence Following Treatment With Collagenase Clostridium histolyticum (CORDLESS [Collagenase Option for Reduction of Dupuytren Long-Term Evaluation of Safety Study]): 5-Year Data. Peimer CA1, Blazar P2, Coleman S3, Kaplan FT4, Smith T5, Lindau T6. J Hand Surg Am. 2015 Aug;40(8):1597-605.
The 5 year results of an a cohort of patients who received collagenase as part of an RCT.
At 5 year follow up of 644 patients, 47% (291) had recurred more than 20 degrees (39% for MCPJ and 66% for PIPJ. 32% (198) had recurred more than 30 degrees (26% of MCPJ and 46% PIPJ).
Of those patients who recurred only 36% opted for further treatment. 47% fasciectomy, 30% collagenase and 23% other interventions.
NICE Guidance
As noted NICE produced guidance for the UK, NHS in 2017 for the website click HERE
DISC RCT
As noted a multicentre RCT was undertaken in the UK in 2017 comparing collagenase and fasciectomy. The trial has a 2 year recruitment and 2 year follow up period with completion planned in October 2021. For further details click HERE
Efficacy and safety of concurrent collagenase clostridium histolyticum injections for multiple Dupuytren contractures. Coleman S1, Gilpin D2, Kaplan FT2, Houston A2, Kaufman GJ2, Cohen BM2, Jones N2, Tursi JP2. J Hand Surg Am. 2014 Jan;39(1):57-64.
This study from 2014 revealed and increase in swelling bruising and minor complication but no increase in major complications or decrease in effectiveness when using 2 vials of collagenase for multiple cords in a single sitting. This would therefore allow patients with multiple fingers affected to be treated in one attendance. The cost effectiveness of this compared with surgery however has not been assessed.
Reference
- orthoracle.com

























