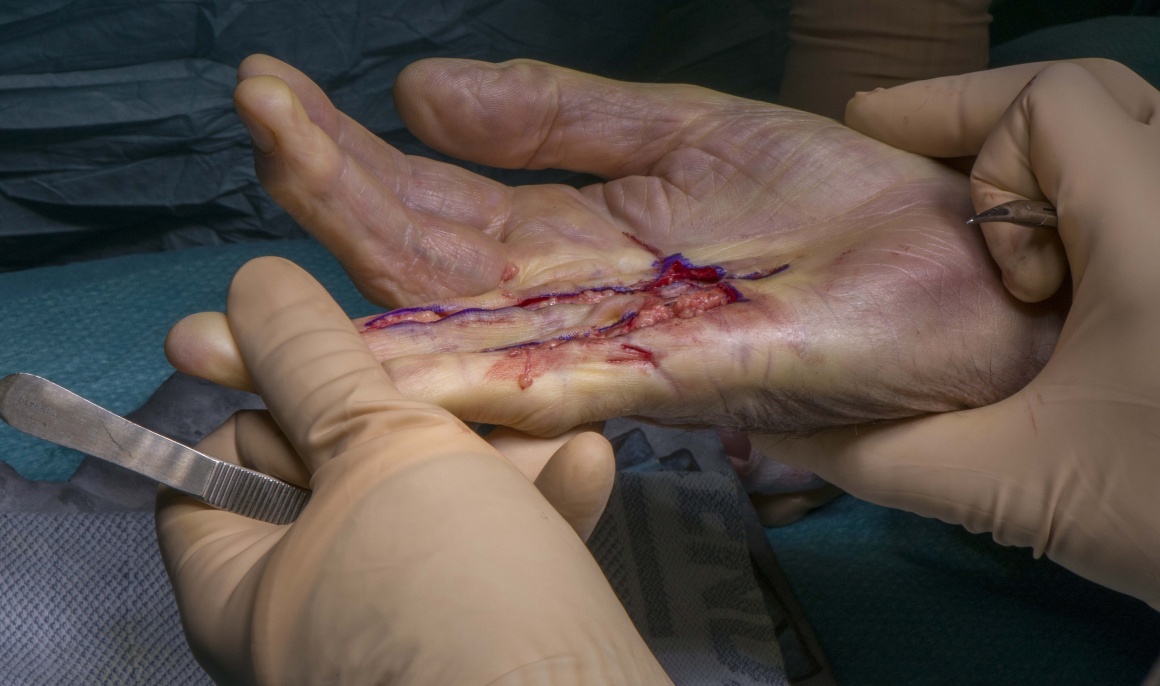
Learn the Dupuytrens contracture: Limited fasciectomy plus Z-plasties surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Dupuytrens contracture: Limited fasciectomy plus Z-plasties surgical procedure.
Dupuytren’s disease is a fibroproliferative disorder affecting the hands. It has a variable clinical course and in most cases it causes contractures of the fingers requiring treatment. The highest incidence of this disease is in the Scandinavian countries, giving it the nickname ‘Viking disease’. It is common in Northern Europe and the incidence decreases towards the Eastern hemisphere. It is very rare in the African and Asian subcontinents. Japan interestingly has a high incidence of Dupuytren’s disease though it appears to be a milder form of disease.
There seem to be genetic and environmental factors involved in the aetiology of this disease. Alcoholic liver disease, anti-epileptic medication, smoking and Diabetes all seem to be risk factors for Dupuytren’s disease. It is commoner in men and the incidence is higher in the fourth and fifth decades of life.
The exact pathogenesis of Dupuytren’s disease is still not clear. There have been several theories about the origin of the disease. One of the theories is that it is a fibrosis of the intrinsic palmar fascia(McFarlane). The other theories are that it is an extrinsic disease which spreads along the palm and fingers(Hueston), or it is a combination of both(Gosset). The most widely accepted theory is that of Murrell which states that there is microangiopathy which releases free radicals which in turn start the fibrotic process.
In 1971, Gabbiani, an Italian scientist discovered a specialised cell called Myofibroblast in Dupuytren’s tissue. This cell is the key to the fibrotic process and has later been discovered in scar tissue.
Dupuytren’s disease can also affect feet, where it is called Ledderhosen’s disease and penis where it is termed Peyronie’s disease. Patients with disease in these ectopic sites have a more aggressive form of disease and it is termed a ‘Dupuytren’s diathesis’.
The decision to treat is made and the treatment method is chosen based on patient’s preference, functional disabilities and pattern of disease.

INDICATIONS: Patients typically present either intrigued by the lumps and in the hand or due to the contractures limiting their function. Indications for treatment is dependent on patient’s functional limitations but generally accepted ones are:
MCP joint contracture more than 30 degrees
Any degree of PIP joint contracture.
Presence of tender nodules in the palm can cause functional problems in certain professions. In these cases a trial of steroid injection into the nodules can be tried. If not successful they can be excised.
There is no indication to treat Dupuytren’s disease without a contracture. The only exception to this may be in patients where radiotherapy is considered as a treatment option. Radiotherapy cannot correct a contracture but can arrest the progression of the disease. The benefit has to be weighed against the potential risks. In patients who have Dupuytren’s diathesis with previous poor outcome to surgery, radiotherapy can be considered in early disease in other fingers.
SYMPTOMS & EXAMINATION
Patients either present intrigued by the lumps and cords in the palm or because the contracture causes them functional problems. As most of the hand function is manageable by the radial side of the hand and Dupuytren’s contracture does not limit flexion of the fingers, patient usually manage quite well with advanced degrees of contracture. The typical patient who presents is a middle-aged Caucasian man who had noticed contractures in the fingers and is starting to have functional problems.
The history is usually of an insidious onset lumpiness in the hand which slowly developed into contractures. The common complaint is of washing the face or putting hands in the pocket. Many patients have a family history of the disease though it is not a well defined inheritance pattern. While taking a history it is important to be systematic and the key points are:
Age, Occupation, handedness and hobbies
Duration of the disease
Functional problems
Other areas of involvement: Feet, penis
Previous treatment
Medical history: Liver disease, epilepsy, diabetes, smoking
Drug history: Anti-epileptic medications
Social history
On examination the presence of lumps and contractures is noted. The affected fingers and the joints as well as the degrees of contractures in noted. Skin involvement and previous scars are noted.Garrod’s pads are looked for on the dorsum and the other hand is inspected. Sensations are noted as well as the range of flexion.
A summary of the clinical problems and a treatment plan is made based on the history and the contractures in various joints.
IMAGING
Dupuytren’s disease is a clinical diagnosis and imaging is not necessary. The only exception is a patient presenting with a fibromatous lump in the hand where a soft tissue sarcoma is suspected and in this case an MRI scan is useful. This however is an extremely rare situation.
ALTERNATIVE OPERATIVE TREATMENT
The surgical treatment options for Dupuytren’s disease are needle fasciotomy where a hypodermic needle is used to perforate the cord which is manipulated and finger straightened, open fasciotomy, where the fascia is divided through a small incision, limited fasciectomy, where the disease causing contracture is excised from the finger, segmental fasciectomy where segments of the cords are excised through small incisions and dermofasciectomy where the skin and cords are excised and a skin graft used to resurface the wound.
NON-OPERATIVE MANAGEMENT
In cases where there are tender nodules in the palm, steroid injection can be used as intralesional injections.
For patients with cords causing contractures, the only non-operative treatment which is useful is collagenase injection, which is an enzyme injected into the cords. The finger is manipulated under local anaesthetic on the following day. Collagenase can be used for MCP and PIP joint contractures and has been shown to be successful in several trials against placebo.
Radiotherapy can be used to stop of the progression of the disease. This however cannot correct a contracture.
CONTRAINDICATIONS
Contraindication to surgical treatment is a patient who is unfit for surgery from co-morbidities. Patients on anticoagulation which cannot be stopped is a relative contra-indication.
Patients with advanced contractures with finger in the palm, are not candidates for fasciectomy. They may be treated by amputation or arthrodesis of the PIP joint in a more functional position.

Limited fasciectomy can be performed under a Brachial block or General anaesthetic. There is a trend towards performing it under local anaesthetic with adrenaline as a wide awake local anaesthetic procedure though this is not my practice.
The arm is positioned on a hand table with an upper arm tourniquet in place. Loupe magnification is essential while doing Dupuytren’s surgery to visualise digital arteries and vessels. The surgeon and assistant are seated on either side of the hand. The hand is positioned on a Lead hand.

The arm is elevated in a sling for 24 hours.
Patients are discharged home the same day.
They are advised to take regular analgesics and to continue elevating the arm.
Patients are reviewed between five to seven days when dressings are changed.
A simple dressing such as Mepore is applied and they are referred to the Hand OTs to have a Thermoplastic splint made. This hand based splint keeps the fingers in extension and they are advised to wear it at night time for the next six weeks. They are advised to mobilise the fingers actively and passively during the day. Patients may have some numbness of the fingers from the dissection of the digital nerves which should settle down over the next four to six weeks.
Sutures are removed at 2 weeks.
At this time patients can resume their normal activities including driving. They are also advised to massage the scar using moisturising cream.
Hand therapy is continued and patients are reviewed at six weeks. At this time one expects to see full flexion of the fingers.
Patients are reviewed again in six weeks to monitor for any recurrence of the contracture or new disease.

Worrell M1.Dupuytren’s disease. Orthopaedics.2012 Jan;35(1):52-60
Dupuytren’s disease is a benign contractile disorder of the hand. The condition commonly affects older men of Celtic descent. Although fibroproliferation and collagen alteration play a role in its etiology, defining a cause remains elusive. Nonoperative intervention for advanced disease has shown only short-term benefit. Therefore, open fasciectomy has become the mainstay of treatment. Associated morbidity and recurrence have prompted investigation into less invasive techniques, including needle aponeurotomy and enzymatic fasciotomy. Data from phase III studies using injectable collagenase are changing treatment algorithms. Postoperative rehabilitation includes night time splinting and immediate active range of motion exercises to facilitate return to function.
Rodrigues JN1, Zhang W2, Scammell BE2, Chakrabarti I3, Russell PG4, Fullilove S5, Davidson D6, Davis TR2 Functional outcome and complications following surgery for Dupuytren’s disease: a multi-centre cross-sectional study. J Hand Surg Eur Vol. 2016 Jul 29. pii: 1753193416660045.
Outcomes 1 or 5 years after an aponeurotomy, fasciectomy or dermofasciectomy were assessed by patient interview and examination at five UK centres. Over 400 procedures were studied. The reoperation rate did not differ at 1 year , but was higher after aponeurotomy in the 5-year group . Loss of function (DASH>15) did not differ between procedures at 5 years, even when reoperation and other variables were controlled. Diabetes, female gender and previous ipsilateral surgery were associated with poorer function . Aponeurotomy had lower complication rates than fasciectomy and dermofasciectomy.
Rodrigues JN1, Becker GW, Ball C, Zhang W, Giele H, Hobby J, Pratt AL, Davis T.Surgery for Dupuytren’s contracture of the fingers. Cochrane Database Syst Rev. 2015 Dec 9;(12):CD010143.
Currently, insufficient evidence is available to show the relative superiority of different surgical procedures (needle fasciotomy vs fasciectomy, or interposition firebreak skin grafting vs z-plasty closure of fasciectomy). Low-quality evidence suggests that postoperative splinting may not improve outcomes and may impair outcomes by reducing active flexion. Further trials on this topic are urgently required.
Reference
- orthoracle.com





























