Learn the Multiple tendon transfers for C8 / T1 loss from spinal infarct: Camitz transfer for opposition; ECRL to FDP for finger flexion; Brachioradialis to FPL for thumb flexion surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Multiple tendon transfers for C8 / T1 loss from spinal infarct: Camitz transfer for opposition; ECRL to FDP for finger flexion; Brachioradialis to FPL for thumb flexion surgical procedure.
Tendon transfers are useful for the restoration of important functional losses. An expendable donor muscle is used for reconstruction of a more useful function. Brand defined the criteria for successful transfer. Each case is unique and the functional deficits should be carefully assessed as well as the strength of potential donors. Patients should be involved in the planning process with pre-operative consultations with the hand therapy team to define the aims of surgery and understand the post-operative rehabilitation requirements.
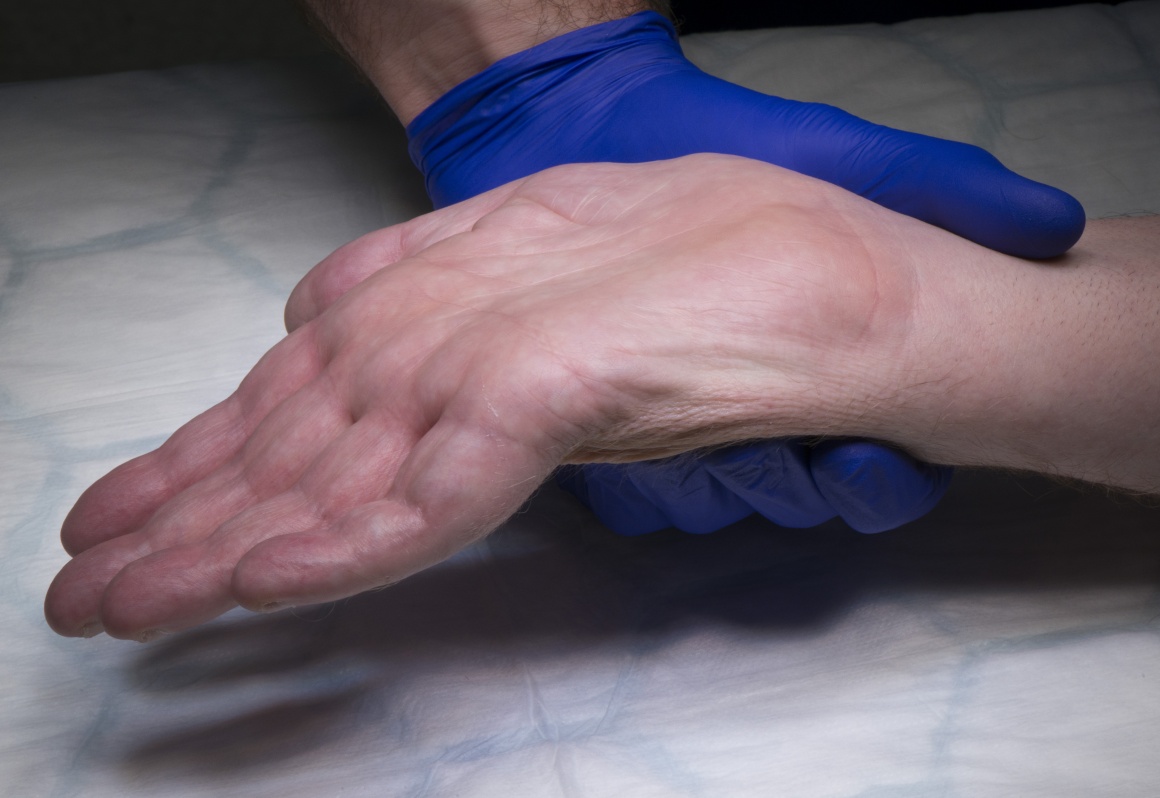
This case is a rare situation where a localised spinal cord stroke has damaged the anterior horn cells and caused a permanent loss of the motor outflow at C8 and T1 unilaterally . This lower motor neurone lesion is not amenable to nerve transfer surgery due to the time elapsed since motor loss. The hand remains supple but functionally useless and the patient wishes to restore some function, but understands that normal function is not possible. The case illustrates the assessment process, the techniques involved in tendon transfer surgery that can be applied to other situations and the rehabilitation following surgery.

INDICATIONS:
Tendon transfers can be used to reconstruct functional loss due to nerve injury, nerve compression, muscle-tendon loss through trauma, post infective paralysis, inflammatory erosion of tendons as is seen in rheumatoid arthritis or congenital absence of muscles and tendons. In the UK, nerve injury reconstruction is the commonest scenario where tendon transfers are undertaken, however worldwide the management of post-infective paralysis from leprosy is the most common reason to consider tendon transfer surgery.
Brand defined the criteria for a successful nerve tendon transfer and these will be discussed later. I would recommend for ease of recollection, when considering the option of tendon transfer it is worth considering criteria in 4 separate categories:
Patient factors:
The cause of paralysis should be known
The deficit must be static
The deficit must be functionally significant
The patient must be able to comprehend the planned treatment and comply with the post-operative rehabilitation requirements
Donor muscle factors:
The muscle should be under voluntary control
The muscle should have MRC grade 4 or greater power
The muscle should have an amplitude of excursion similar to the recipient tendon
The muscle should be phasic with the function of the muscle to be reconstructed
Surgical bed factors:
Definitive surgery for the skeleton should be completed
Absence of infection
There should be minimal scarring in the bed for the rerouted tendon
Tendons should be rerouted subcutaneously when possible
If a change of direction is required for the vector of pull then a pulley must be created
Target factors:
The joints to be moved should be supple
The joints should be stable
The skin should be sensate (not always necessary – NB Leprosy)
Direct transfer with overlap of donor and recipient tendon to allow a robust repair – otherwise an interposition tendon graft is required
In this case the spinal stroke resulted in lower motor neurone paralysis of the muscles innervated by C8 and T1 with relative sparing of proximal C5, C6 and C7 innervated muscles. The deficits resulting are similar to those seen in a lower trunk injury of the brachial plexus with loss of digit flexion and intrinsic function. Digit extension is preserved in this case through C7.
SYMPTOMS & ASSESSMENT:
The history and examination should identify the cause of the deficit and confirm that the deficit is static. A functional assessment and review by a hand therapist will help to identify the optimum tendon transfer possibilities. Donor muscle strength should be carefully assessed and documented. Consideration should be given to whether the donor muscle is expendable. In cases of paralysis patients may use functional adaptation of existing muscles to compensate for the missing function.
The flexibility and stability of the target joints should be assessed.
The sensation of the target skin should be examined using 2 point discrimination and monofilament pressure threshold assessment.
Te surgical bed should be assessed for scarring in the line of the tendon transfer and if necessary soft tissue corrective surgery (metalwork removal, skin graft excision, flap resurfacing) should be considered where the tendon transfer will lie in advance of any reconstructive surgery.
INVESTIGATION:
Radiographs may be necessary to confirm underlying fracture healing.
Neurophysiology studies may be used to confirm that there is no recovery to be expected in the target muscle function and to assess the quality of the donor muscle in uncertain cases such as brachial plexus injuries where a recovered muscle may be used as the donor for transfer.
A pre-operative assessment with a hand therapist is essential to help the patient understand the aim of the surgery, prepare for surgery by optimising the donor function and to anticipate the post-operative regimen, splint age and retraining requirements. The therapist will be able to provide tailored advice regarding activities of daily living and task performance during the recovery phase.
OPERATIVE ALTERNATIVES:
Nerve transfers are a viable alternative to tendon transfers in isolated peripheral nerve injuries. Nerve transfer surgery involves the re-innervation of the denervated muscle using an expendable motor branch (nerve transfer) or redundant motor fascicle from within a mixed motor-sensory nerve between motor branch points (highly selective fascicle transfer). The benefits of nerve transfer include re-innervation of the original muscle in tis original bed without change of sarcomere resting length or disturbing the vector of pull. In addition there is no alteration to amplitude of excursion. Control of the newly innervated muscle is achieved through neural plasticity and is optimum is cases where a phasic nerve is use for the transfer (for example a wrist flexor is used for finger extension; a wrist extensor is used for finger flexion). In this case nerve transfer is not possible due to the longstanding nature of the denervation from this lower motor neurone lesion. there is Wallerian degeneration and the motor end plate degeneration and collapse of the intramuscular neural network renders the muscle unreceptive to axonal ingrowth after approximately 9-12 months. In upper motor neurone lesions as seen in some muscle groups below the level of a narrow segment spinal cord injury in the tetraplegic upper limb, there may be preserved neural pathways between the spinal cord and the muscle. In this specific scenario the use of a donor nerve or fascicle under volitional control from above the injury directed to a muscle below the injury may be successful beyond 12 months because denervation only commences from the moment of the nerve transfer. These techniques will be discussed elsewhere in OrthOracle.
NON-OPERATIVE ALTERNATIVES:
Functional splints may assist weak muscles or improve the posture of the hand such that preserved muscle function may be optimised. Robotic exoskeletons may be of use in the flail limb for functional assistance. However currently these devices are expensive and not widely available.
CONTRAINDICATIONS:
Tendon transfer surgery should not be contemplated in progressive motor paralysis seen in motor neurone disease (amyotrophic lateral sclerosis – ALS) and should be used with caution in disease processes which have stepwise deteriorations over many years (multiple sclerosis, spinal muscular atrophy, hereditary sensory motor neuropathy). In such cases the gains from tendon transfer surgery are likely to be subsequently lost. There are scenarios where function can be improved, for example in case where there is extremely limited function, arthrodesis of the wrist may allow a functional wrist extensor to be used for transfer to finger flexors to enhance the functional status of the limb. I have used this technique in spinal muscular atrophy where no other function existed below the elbow.

The patient uses regular anti-platelet therapy. This must be stopped prior to surgery and the need for bridging anticoagulation to cover the peri-operative period should be discussed with a haematologist.
The operation is performed under a regional anaesthetic block at the axillary level. An upper arm tourniquet is applied to achieve a bloodless surgical field. I recommend preparation of the whole limb and then use of a sterile tourniquet and an Esmarch bandage for exsanguination. This reduces the ischaemic time and makes it possible to perform this procedure under a single tourniquet application.
Tendon transfer instruments are essential for this procedure. The tendon passer allows retrieval of tendons through small subcutaneous tunnels and the tendon weave instruments allow completion of a Pulvertaft weave with ease.

Following surgery the arm should be elevated in a high Bradford sling and the patient should be advised that elevation should continue during the first 2 weeks following surgery to reduce swelling, prevent wound healing problems and improve tendon glide.
The patient should be prescribed analgesic medication and advised to start using medication when the first sensation starts to return to the fingers. Analgesic use should continue as required and is advised prior to dressing changes and hand therapy sessions to ensure maximum tendon glide without pain inhibition.
The cast should be removed at 2 weeks and suture removed. At this stage thermoplastic splint can be applied to the limb with elbow extension block for two weeks then a final two weeks with forearm wrist and hand dorsal block thermoplastic splint only. Tendon gliding exercises should be commenced with a hand therapist at 2 weeks and continued throughout the period of immobilisation.
Weaning from the splint commences at six weeks with night weaning from eight weeks and work hardening exercises from 8 weeks.
If the recruitment of the PL to AbPB tendon transfer is poor, a thumb abduction / opposition hand-based splint can be fitted to allow functional use of the thumb and finger flexion transfers.

Tendon transfers are a reliable method of restoring function to the paralysed hand. Brand’s criteria help in decision making and adherence to these criteria helps to ensure good functional outcomes. Donor muscles should be tested to ensure that they are of sufficient strength and the joints in the digits to be mobilised should be stable and supple. The patient must understand the rehabilitation programme and the goals should be clearly pre-defined. The donor and recipient matching is important and movements should be phasic wherever possible. Wrist extensors are suitable for finger flexors however the excursion of the respective tendons are slightly different resulting in failure to restore full digit roll up. The use of tenodesis to improve tension in the transfer can help to improve this amplitude mismatch.
1: Brand PW. Biomechanics of tendon transfers. Hand Clin. 1988 May;4(2):137-54
2:Brand PW, Beach RB, Thompson DE. Relative tension and potential excursion of muscles in the forearm and hand. J Hand Surg Am. 1981 May;6(3):209-19
3:Brand PW. Biomechanics of tendon transfer. Orthop Clin North Am. 1974 Apr;5(2):205-30
4: Brand PW. Tendon transfers for median and ulnar nerve paralysis. Orthop Clin North Am. 1970 Nov;1(2):447-54
5: An KN, Linscheid RL, Brand PW. Correlation of physiological cross-sectional areas of muscle and tendon. J Hand Surg Br. 1991 Feb;16(1):66-7
6: Rymer B, Thomas PB. The Camitz transfer and its modifications: a review. J Hand Surg Eur Vol. 2016 Jul;41(6):632-7
7: Cooney WP. Tendon transfer for median nerve palsy. Hand Clin. 1988 May;4(2):155-65































































































