Learn the Open Reduction Internal Fixation of a Monteggia forearm fracture dislocation using the Synthes small fragment LCP plate surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Open Reduction Internal Fixation of a Monteggia forearm fracture dislocation using the Synthes small fragment LCP plate surgical procedure.
A Monteggia fracture-dislocation is a fracture of the proximal one third of the ulna and an associated dislocation of the radial head and is named after Giovanni Battista Monteggia who described it in 1814. Monteggia fractures are thought to occur from a fall on to a hyper-pronated forearm / hand. They are relatively uncommon with an incidence of between 1% to 2% of all forearm fractures. They are more frequently seen in children compared to adults however, the literature and treatment options must be interpreted with caution as the groups are often mixed together.
The forearm comprises two bones (radius & ulna) that are held together at different levels by different soft tissue structures. Distally the forearm is connected at the Distal Radio-Ulna Joint (DRUJ) by the Triangular FibroCartilage Complex (TFCC). In the mid-portion the bones are connected by the interosseous membrane and proximally the radius is held by the annular and quadrate ligaments. The annular ligament arises from the anterior and posterior aspects of the radial notch in the proximal ulna. The annular ligament is a strong band of fibres that encircle the proximal radius, maintaining its position in the radial notch but also allowing it to freely rotate during supination and pronation. The quadrate ligament arises from the inferior border of the radial notch on the ulna and connects directly to the radial neck. Its’ function is to increase the stability of the Proximal Radio-Ulnar Joint (PRUJ) and restrict excessive supination / pronation.
The Synthes Locking Compression Plate (LCP) has uniformly spaced combination (combi) holes. The plate can be applied in any of the following modes:
Compression
Bridging
Neutralisation
Buttress
Tension band
The combi holes can accommodate standard cortical / cancellous screws and locking screws. The combi holes are a mirror image relative to the middle of the plate. This places the threaded hole section (for locking screws) closer to the fracture and the dynamic compression unit (DCU) side of the hole is furthest away from the fracture. This means that with eccentric cortical / cancellous screw placement, then compression is achieved at the fracture site.
As the plates allow the insertion of locking screws, this converts the construct into a fixed angle device and you do not need to rely on plate/bone compression to maintain the stability of the construct.
The small fragment LCP plates will accept the following screw sizes:
3.5mm cortical screws
4.0mm cancellous screws
3.5mm locking screws

INDICATIONS
In adults, all Monteggia fractures should be treated surgically with an anatomical reduction and stabilisation of the ulna, this usually reduces the dislocated radial head.
SYMPTOMS & EXAMINATION
A forearm fracture is usually very painful and this type of fracture often results in a very swollen elbow with a restriction of movement. There will be swelling and sometimes bruising. Rarely a forearm compartment syndrome may develop.
An examination will reveal limited elbow movement which is very painful. A hand examination is essential and you must thoroughly examine and document the findings. The autonomous zones for the peripheral nerves are:
Radial (dorsal 1st webspace)
Median (index finger pulp)
Ulnar (little finger pulp).
To examine the motor component of each nerve, ask the patient to place the hand palm downwards:
Extend the wrist (radial nerve)
Extend the fingers (PIN: posterior interosseous nerve – terminal branch of the radial nerve)
Abduct the fingers (ulnar nerve)
Turn the hand palm upwards and abduct the thumb (median nerve)
Form an ‘OK’ sign (AIN: anterior interosseous nerve – terminal branch of the median nerve).
This injury can cause an isolated injury to the PIN due to its proximity to the proximal radius.
IMAGING
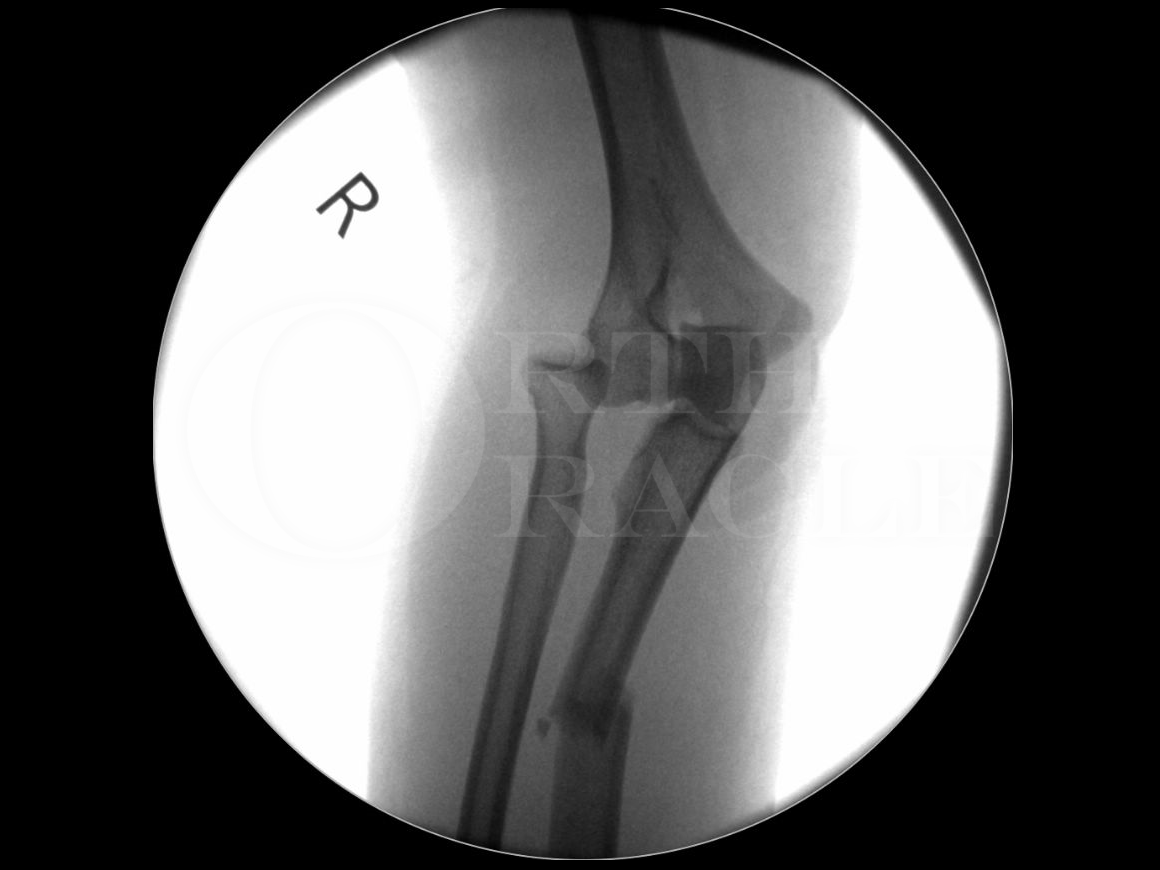
Plain X-Rays of the elbow, Antero-Posterior (AP) and Lateral (Lat), are usually sufficient to make the diagnosis.
In the acute injury MRI has no role. A CT scan however may be useful as it might reveal another occult injury (e.g. radial head fracture, coronoid fracture) or can be used to clarify these if there is anything suspicious on the plain imaging.
ALTERNATIVE OPERATIVE TREATMENT
In adults an ulna fracture requires anatomic reduction and rigid stabilisation. This is usually sufficient to reduce the dislocated radial head.
If there is a displaced radial head or coronoid fracture, these should also be treated with open reduction and internal fixation. Occasionally an un-reconstructable radial head fracture will require replacement. This is important if there is longitudinal instability of the radius, as this can lead to an Essex-Lopresti type DRUJ pathology or ongoing elbow instability, as the radial head is a primary stabiliser. Radial head replacement for this indication can also be read on OrthOracle Radial Head Replacement Using Evolve Proline Modular Radial Head System (Wright Medical)
In children, often a simple manipulation under anaesthetic and application of an above elbow plaster of paris is sufficient. Alternatively the ulna can be stabilised with an elastic nail.
NON-OPERATIVE MANAGEMENT
For any forearm fracture that disrupts the axis of rotation (supination / pronation) non-operative management is not recommended. The forearm axis of rotation is from the centre of the radial head to the centre of the ulna head. If the axis is disrupted, this means that there will be a consequent loss of forearm rotation which can lead to significant disability. It should only be considered if surgical treatment is not possible.
CONTRAINDICATIONS
The only contraindications for surgical fixation are:
Infection
Large soft tissue defects requiring delayed reconstruction
Anaesthetic (general / regional) contraindications

A large number of surgeons would choose to operate with the patient in a lateral position with the patient’s arm over an appropriately padded rest or gutter.
An alternative technique is to have the patient supine with the arm flexed up over the patient’s chest. Often a pillow on the chest is helpful to prevent over-flexion of the elbow which displaces the reduction and the pillow also provides some protection for the chest. The patient’s axilla must rest on the edge of the operating table, as this will give enough room to bring in the C-arm and have the elbow in the centre of the detector. In this case, the patient had multiple rib fractures, so was kept in a supine position.
Intravenous antibiotics are administered.
A tourniquet is applied and inflated to 250mmHg. I do not exsanguinate the limb using either an Esmarch bandage or Rhys Davies exsanguinator. I simply elevate and gently squeeze to allow the veins to collapse but still contain some blood, so that I can see them and then haemostases them if required. Some surgeons prefer to use a sterile tourniquet however, as we are not extending the incision above the elbow, I do not feel this is necessary.
The other benefit of the supine position is if the radial head needs reconstruction, then an arm table can be used.

Distal neurovascular assessment:
If placing the plate on the dorsal surface of the ulna, you should avoid the ulna nerve which is on the medial side of the elbow.
The posterior interosseous nerve also needs to tested, as the dislocated radial head can cause an isolated injury to this nerve.
Immediate gentle elbow range of motion exercises (flexion / extension, and supination / pronation). No heavy lifting or loading of the forearm / elbow for 6 weeks or until signs of union.
When attending the clinic at 2 weeks post-op:
X-ray on arrival to check the fracture and radial head reduction
Wound inspection +/- removal of any sutures
Discontinue using a sling (if wearing one) and strongly encourage range of motion exercises.
Referral to physiotherapy and forewarn the patient that they will lose some elbow range of motion but that they must work hard early on to minimise this.
Further follow up in 4 weeks and then at 6 week intervals with x-rays at each attendance until the fracture has united (or is making satisfactory progress towards union).

In 1955, Watson-Jones noted only 2 good results among 34 Monteggia fracture-dislocations in adults. Earlier he had stated that “no fracture presents so many problems; no injury is beset with greater difficulty; no treatment is characterised by more general failure”.
Ring et al. noted that posterior Monteggia injuries have higher rates of recurrent instability and worse outcomes compared to the more predictable anterior dislocation injuries.
In a paper by Klug et al. they retrospectively reviewed their series of Monteggia-like lesions i.e. a proximal ulna fracture and an associated radial head fracture. They concluded that treatment of the coronoid and radial head fracture were required to provide elbow stability. In their opinion, all Mason type II and III fractures amenable to reconstruction should be rigidly fixed and good outcomes can be achieved.
In non-reconstructable injuries, without ligamentous instability, a radial head replacement did not provide better outcomes compared to radial head excision at mid-term follow up (4.6 years). However, if there were a ligamentous injury then radial head replacement was indicated to allow functional rehabilitation.
Watson-Jones R. Injuries of the forearm. In: Fractures and joint injuries. 4th Edition. Baltimore (MD): William and Wilkins; 1955. 572-81
Ring D, Jupiter JB, Simpson NS. Monteggia fractures in adults. J Bone Joint Surg Am. 1998; 80(12): 1733-44
Klug A et al. Surgical treatment of the radial head is critical to the outcome of Monteggia-like lesions. Bone and Joint Journal 2019; 101-B: 1512-19
Reference
- orthoracle.com















































