Learn the Posterior interosseous nerve decompression surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Posterior interosseous nerve decompression surgical procedure.
The posterior interosseous nerve (PIN) is a terminal branch of the radial nerve and supplies innervation to the extensor carp ulnaris (ECU) and the digital extensors. The PIN passes through the supinator tunnel to enter the dorsal forearm. The supinator tunnel is formed by the two heads of the supinator. The superficial head of supinator arises from the lateral epicondyle of the humerus and the deep head from the supinator crest of proximal ulna. The two muscle heads converge as they encircle the proximal radius and they form a common tendon that inserts to the radius shaft distal to the bicipital tuberosity. The nerve passes between the two heads. The PIN is in contact with the bone of the radius neck, but the deep head separates if from the radius shaft within the mid and distal thirds of the supinator tunnel. If the nerve is entrapped in the supinator tunnel patients present with dorsal forearm pain, worse with activity, limited digit extension and radial deviation of the wrist due to loss of the ECU’s stabilising effect on the pull of the extensor carpi radialis longus.
The common sites of entrapment are the leash of Henry (radial recurrent vessels) and the arcade of Frohse (proximal fibrous brach of the supinator). The nerve branches within the tunnel and at the distal end, as it emerges in the dorsal forearm it lies in close proximity with the posterior interosseous artery and gives branches to the ECU, EDC and EDM muscles. The remaining PIN passes distally and provides branches to the APL, EPB, EPL and finally the EIP muscles.
The nerve should be imaged in the tunnel to exclude intrinsic nerve tumours or extrinsic causes of nerve compression. The condition may be associated with proximal radio-capitellar synovitis and can also be of spontaneous onset with a viral inflammatory aetiology.
Decompression o the PIN in the tunnel may prevent further deterioration and salvage residual function in the posterior interosseous nerve, preventing further loss of digit extension.
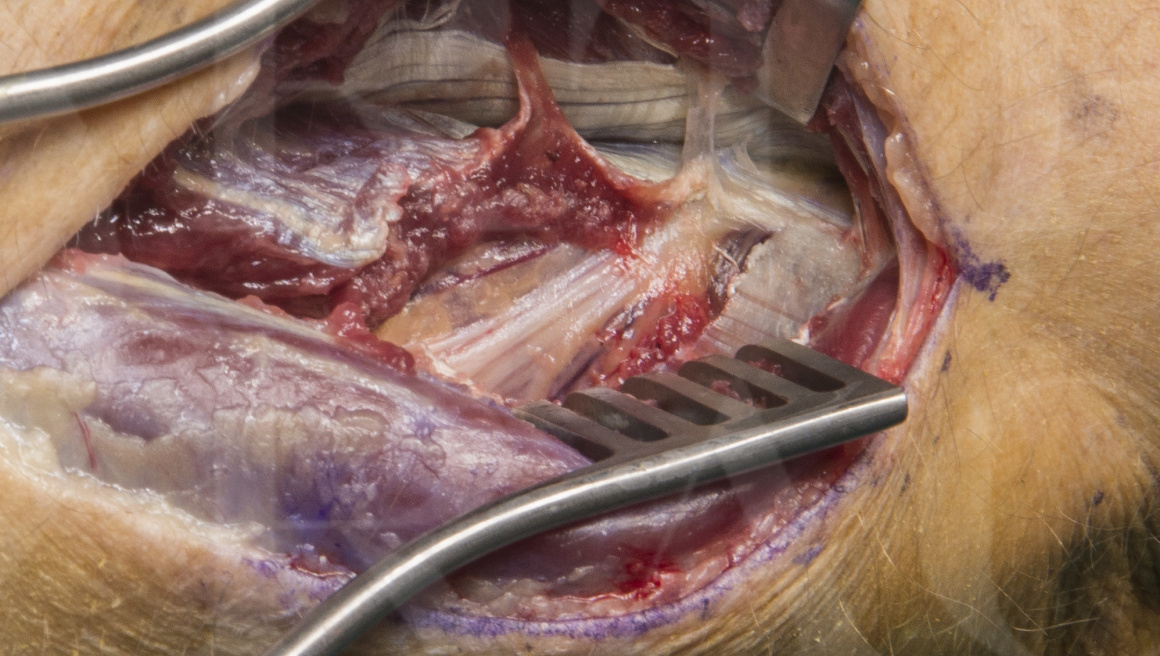
The case illustrated had spontaneous onset of proximal dorsal forearm pain and loss of finger extension with normal imaging studies of the neck and he posterior interosseous nerve. Clinical examination demonstrated weakness in the PIN innervated muscles at MRC grade 2 that had persisted without recovery for three months. There was proximal tenderness over the proximal supinator and the PIN dorsally. Electromyography demonstrated partial chronic denervation of the PIN innervated muscles with intact function of the flexor carpi unlearns, suggestive of pathology at the level of the PIN and not more proximally at the C8 nerve root.

INDICATIONS
The posterior interosseous nerve (PIN) is one of the terminal branches of the radial nerve. At the lateral elbow the PIN and the superficial radial nerve (SRN) branch from the radial nerve. The extensor carpi radials brevis (ECRB) branch is variable in origin and sometimes arises from the SRN and sometimes from the PIN. The first branches of the PIN are the medial and lateral supinator branches. These leave the main nerve prior to reaching the supinator muscle. The supinator has two heads (humeral and ulnar). The PIN passes into the forearm between the two heads and is closely related to the proximal radius throughout the first 1/3 of the forearm. The PIN passes radially around the radius to lie on the posterior aspect of the interosseous membrane in the forearm. The nerve is at risk during surgery on the proximal radius, particularly for biceps tendon reattachment, fracture fixation and the management of radial head dislocation. The posterolateral approach to the radial head recommends pronation of the forearm to move the PIN anteriorly, away from the surgery site. During a volar approach to the proximal radius, full supination moves the nerve away from the site of surgery and in a lateral direction.
The PIN branches within the tunnel and at the distal margin of supinator there are branches to EDC and ECU. The EDM branch arises next, then further down the forearm the main PIN trunk branches to EPL, EPB, APL and finally to EIP. There are branches of the terminal PIN that provide innervation to the wrist joint.
SYMPTOMS & EXAMINATION
PIN entrapment is associated with weakness of finger and thumb extension with dorsal forearm pain that may be exacerbated by repeated digital extension and resisted supination in the extended elbow position. The cause can be an entrapment neuropathy within the supinator muscle. This explains the common pain exacerbation with supination. The proximal radioulnar joint (PRUJ) may also be a source of synovitis and secondary irritation and compression of the PIN. This is often associated with rheumatoid arthritis. Other causes of PIN dysfunction can be related to a post viral inflammatory neuropathy, intrinsic nerve tumours or extrinsic tumours causing compression of the PIN.
The differential diagnosis is either a C8 nerve root compression which can mimic the digit extension weakness, or rupture of the extensor tendons associated with distal radioulnar joint (DRUJ) arthropathy. In the latter case there will be a loss of the normal tenodesis enabling passive digital extension when the wrist is flexed plus some deformity, loss of motion and crepitus at the DRUJ.
IMAGING AND NEUROPHYSIOLOGY STUDIES
Imaging the PIN with ultrasound (US) or magnetic resonance imaging (MRI) can identify other causes of pathology and assist with surgical planning. Imaging of the cervical spine with MRI may exclude a compressive lesion of the C8 nerve root. Plain radiographs may identify pathology at the elbow and in particular erosive or deforming arthropathy associated with rheumatoid arthritis.
Neurophysiology evaluation should include electromyographic (EMG) assessment of the PIN innervated muscles. Active denervation with increased insertional activity, fibrillation and positive sharp waves are features of an acute lesion with ongoing Wallerian degeneration. Chronic lesions may have low amplitude, evidence of polyphasic responses from reinnervation and giant motor units. Sampling of non-PIN innervated C8 muscles (typically the flexor carpi ulnaris) will confirm denervation in this muscle if the pathology is at the level of the C8 nerve root due to a motor radiculopathy of C8. Sensory conduction velocities are not useful as the PIN is motor with proprioceptive fibres from the wrist and afferent fibres from the PIN innervated muscles and tendons. Sensory conduction velocity abnormality in the superficial radial nerve territory can confirm that the lesion is a high radial palsy and in such cases EMG of the ECRL and BR would confirm denervation changes in these muscles.
ALTERNATIVE OPERATIVE TREATMENT
The PIN may be decompressed through a volar approach, a dorsolateral approach or a direct approach through the mobile wad muscles.
My preferred technique is to use a volar approach when the proximal supinator (arcade of Frohse) or the radial recurrent vessels (leash of Henry) are thought to be the source of compression. The volar approach is also indicated when a nerve transfer is contemplated from the supinator branches (SPIN transfer) or from the median nerve (typically FCR and PL fascicles from the median nerve to the PIN in high radial nerve palsy).
When there is an associated lateral epicondylitis, the ECRB tendon must be released and the lateral approach between BR and ECRL or the dorslateral Thompson approach between ECRB and EDC may be a superior approach. The Thompson approach is also indicated when the pathology lies within the distal supinator.
NON-OPERATIVE MANAGEMENT
In the early phase of PIN entrapment a period of conservative management with rest and activity modification is to be recommended. During this phase the imaging and neurophysiology studies can be completed. Review after an interval of 6 weeks will confirm that the condition is not resolving spontaneously and therefore surgery can be planned.
CONTRAINDICATIONS
There is a relative contraindication to exploration and decompression of the PIN in a longstanding lesion where there is no residual function on EMG testing and chronic muscle denervation changes. In such cases the patient may be better treated with tendon transfer reconstruction for the paralysis of the digit extensors.

The patient is anaesthetised either with a general anaesthetic without neuromuscular paralysis, or a regional anaesthetic block proximal and remote from the site of surgery. The type of anaesthesia should allow intra-operative neuromuscular stimulation to determine response to decompression and the quality of retained function within the PIN. The stimulation can assist in providing an accurate prognosis and in planning the timing of any salvage interventions with tendon transfer reconstruction for severe paralysis.
A well padded pneumatic upper arm tourniquet is used to provide a clear operative field. There are many small blond vessels that need careful dissection and ligation during this exposure and without a tourniquet there is the risk of bleeding obscuring the view of the PIN and its many fine branches.
Basic hand instruments are required for the procedure. A Gemini or Mixter fine tipped 90 degree jawed forceps are useful for passing and retrieving surgical rubber loops that are passed around the nerve for retraction and ease of dissection. The rubber loops avoid excessive traction and inadvertent injury to the nerve branches.
A nerve stimulator is an essential component of the surgery. I use a standard stimulator box that is available for nerve identification and stimulation during regional anaesthesia. I use a nerve stimulator needle that is wrapped in an arthroscopic camera drape and a circuit is completed with a remote electrode outside the sterile surgical field. The box is controlled by the circulating theatre staff and the needle can be unsheathed and rested against the nerve under test by the operating surgeon. The needle is bevelled and care must be taken to avoid injury to the nerve under test.

The arm is monitored for swelling before discharge the same day as the operation.
The patient is encouraged to start to use the hand functionally and to perform gentle range of motion to allow full supination and pronation as soon s the regional anaesthetic block has worn off.
Lifting and strenuous activity should be avoided in the first two weeks as it will cause pain around the surgery site.
The bulky outer dressings are reduced at 5 days and the wound is inspected and redressed.
the wound should be kept clean and dry for 12 days after the surgery.
A clinical review at 6 weeks and 3 months are planned to monitor for any neurological recovery.

The results of PIN decompression are dependent on the underlying pathology, the severity or compression and the duration of the compression.
In this case the decompression resulted in rapid recovery of MRC grade 4 power of digit extension by 6 weeks and a strong MRC grade 4 by 3 months. The denervation on the pre-operative EMGs means that a full recovery to MRC grade 5 power may not be likely.
The published literature on PIN compression is less clear than for more common entrapment neuropathies like carpal tunnel or cubital tunnel. The limited literature and difficult interpretation also reflects the uncertainty in aetiology.
The paper by Ng et al. reports that PIN syndrome may be due to mechanical compression of the nerve or inflammatory neuropathy and recommends imaging to exclude a compressive aetiology. Decompression should be undertaken when there is a mechanical compression and a period of observation for 6 weeks prior to decompression is recommended in cases where there is a presumed inflammatory aetiology.
The paper by Does et al. reviews 6 series in which decompression has been performed but comments that there is an inclusion bias in that there are no high quality conservative observation studies reporting on clinical outcome following compression.
The paper by Totama et al. reports on 38 PIN palsies treated and suggests that there is a tendency to greater function with interfascicular neurolysis in younger patients and older patients with less than 7 months of paralysis. The paper recommends in younger patients with paralysis of 12 months or more and in all patients over 50 years of age with greater than 7 months, that an internal neurolysis should be supplemented with tendon transfers.
Tendon transfers are the main treatment strategy for longstanding paralysis and the results are good. Wrist extension is maintained with the ECRL and the typical tendon transfer for digit extensors is the FCR with Pl for thumb extension. FCU is not recommended for digit extension due to the pre-existing unbalanced radial deviation from loss of the ECU function.
References:
Management of atraumatic posterior interosseous nerve palsy. Sigamoney KV, Rashid A, Ng CY. J Hand Surgery Am. 2017 Oct;42(10):826-830
Interventions for treating the posterior interosseous nerve syndrome: A systematic review of observational studies. Huisstede BM, Miedema HS, vanOpstal T, de Ronde MT, Kuiper Ji,Verhaar JA, Does BW. J Peripher Nerv Syst. 2006 Jun;11(2):101-110
3. Surgical treatment of spontaneous posterior interosseous nerve palsy: A retrospective study of 50 cases. Ochi K, Horiuchi Y, Tazaki K, Takayama S, Nakamura T, Ikegami H, Matsumura T, Toyama Y. J Bone Joint Surgery Br. 2011 Feb;93(2):217-22
Reference
- orthoracle.com


































