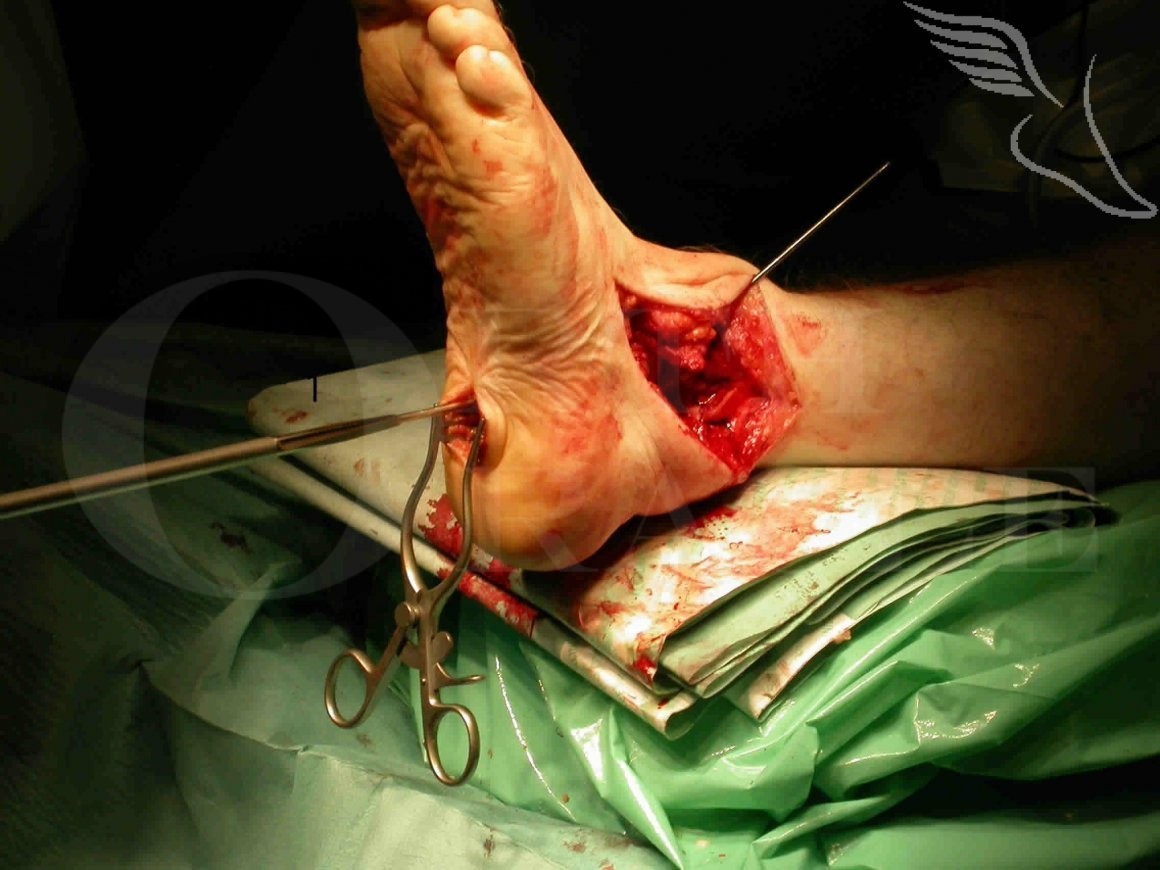
Learn the Double fusion (Tibiotalocalcaneal fusion) with De Puy Versa-Nail surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Double fusion (Tibiotalocalcaneal fusion) with De Puy Versa-Nail surgical procedure.
The fixation of a double fusion using an intra-medullary nailing technique is one of the commoner options utilised for combined Ankle and Subtalar degenerative change with or without deformity. It is a technique that should also be considered in revision ankle fusion cases without Subtalar arthritis and neurological cases presenting with ankle and hindfoot instability rather than deformity.
In the correct patient (and using intra-medullary nail fixation) early load bearing may be achievable. Union rates in many published series are in excess of 90%.
It can however be a technically challenging and relatively long operation to perform.
The implant technique detailed is for the De Puy Versa-nail but the preparation of the arthrodesis described is the same irrespective of the implant type and to a large extent the technique also. A number of the technical details relating to the required steps during intra-medullary nailing are also shared with other nailing systems.

INDICATIONS:
Combined severe Ankle & Subtalar osteoarthritis: This may be with or without deformity. In the presence of deformity it is key to identify accurately where the deformity lies so it can be fully corrected. This is best defined with CT or MRI.
Revision Ankle Fusion: In the presence of isolated Ankle arthritis that has failed to unite with an appropriate technique argument can be made for increasing the rigidity of the construct used for the second operation by using a nail and fusing both ankle and subtalar articulations. It is also a useful way of stabilising across areas of bony loss (prior to packing with bone graft).
Severe Ankle Arthritis with mild subtalar arthritis: This indication is more of a balancing act . The functional outcome after isolated ankle fusion is likely in most to be less restricted than after a double fusion, especially with a mobile subtalar joint. If there is some subtalar arthritic change already and this progresses after the isolated ankle fusion then it is well recognised that a subsequent secondary subtalar fusion will have a lower chance of success than one done as a primary operation together with the ankle fusion .
Ankle & Hindfoot deformity in the adult neurological patient: Most commonly this is an unstable & varus ankle +/- subtalar joint ,with or without arthritic change .
SYMPTOMS & EXAMINATION:
Most patients with severe ankle & subtalar arthritis localise the pain well to the joints. Very much as with arthritis elsewhere symptoms tend to progress from early activity /start up pain which eases off through to progressively more disabling and continual weight bearing pain and on occasion as far as pain at night or at rest. A much less common symptom which can co-exist with pain is that of ankle and hindfoot instability.
The vast majority of patients will either have a history of a significant injury, chronic deformity (for example Cavo-varus) or a past history of untreated chronic lateral ligament instability. With arthritis of both ankle and subtalar joints the possibility of an inflammatory arthropathy should bear proper consideration.
On examination swelling and tenderness localised to the ankle and hindfoot is common. Range of movement is often reduced and may be uncomfortable. Any deformity should be noted. Varus is most common and valgus and equinus less common. The key issues with any deformity are A:Whether it is passively correctable (or not) and B.:Being sure of its anatomical location(s). The former is easily clinically determined .The latter can be more difficult to be sure on , in particular in the presence of severe deformity and CT is indicated for this.
In assessing equinus it should be appreciated at what level(s) the deformity rests. Beware of associated fixed midfoot equinus which will leave the mid/forefoot in a plantar flexed position once the ankle is fused in neutral if it is ignored. A midpoint plantar fascia release may be all that is required to place the foot in a functional position post-operatively. If dealing with isolated ankle equinus be prepared to add a triple cut (or open )Achilles release dependent on the severity of the deformity. With an open ankle fusion often enough laxity is created in the soft tissue envelope by the bone preparation to allow correction of the equinus.
In neurological cases the 1st ray may be disproportionately plantar-flexed and may require a dorsiflexing osteotomy in isolation .
The foot must be in functional and plantar-grade position at the end of the double fusion and on occasion this may require extension of the fusion into the taol-navicular and Calcaneo-cuboid joints , to rotate and stabilise the foot into a functional position .
The rest of the lower limbs alignment should not be forgotten. In general correction of deformity should start proximally and proceed distally. A varus and arthritic knee should be corrected and replaced before the ankle is fused .
A vascular examination must be made and if abnormal dealt with appropriately.
INVESTIGATION:
There are certain factors which need specific consideration if one is using intra-medullary fixation for a double fusion as opposed to using plates ,screws or a frame. The main one perhaps is that the distal Tibial Diaphysis needs to be wide enough anatomically to accept a Nail .This is best measured from a CT if equivocal. Also there should be minimal or ideally no angular deformity within the lower tibia. If there is ,in particular in the post-traumatic case , then nailing may be precluded (or a short nail may be required).
Plain X-Ray: This is the initial imaging for most patients with ankle and subtalar arthritis of any degree. Though the ankle is relatively well visualised (and the films should be taken weight-bearing) the subtalar and midfoot joints aren’t so well shown , in particular in the presence of associated deformity through the area.
CT scan. This is better in defining how much significant arthritic change exists and where it is than MRI . It is also easier to differentiate the level of deformity from a CT than an MRI . There are cases where significant cystic change exists and will require bone grafting.Its location and extent is again best defined with CT. On occasion the use of structural bone graft to reconstruct deformity may be required .The amount may go beyond what can be harvested from the excised Fibula and planning the requirement for femoral head allograft is a call that is often easier to make from a CT scan.
MRI scan: An MRI is more sensitive for early degenerative change but will be degraded by any internal fixation and though sensitive is not 100% sensitive for early arthritis. It can be more difficult to be objective about the severity of more advanced arthritic change as bone oedema ( a reversible phenomenon which can be present in healthy periarticular bone) complicates the MRI images. A CT lacks this sensitivity. Some surgeons prefer MRI to CT in assessing a joint pre-fusion and this is absolutely legitimate.
ALTERNATE OPERATIVE TREATMENT:
Before commencing a nailing procedure for a double fusion it is wise always to have a back-up plan and alternate form of fixation available which one is used to. For a nailing to succeed the Calcaneus must have been placed operatively beneath the Tibia (to allow a straight line of approach for reaming and nail insertion) , any existing fixation that interferes with nail placement must be removable and the intramedullary dimensions of the Tibia in particular need to be adequate (or be reemable to adequate dimensions) to accept the nail. Though an uncommon occurrence on occasion a nail is not passable for one of these reasons.
Alternate forms of fixation are a combination of large fragment screws ,compressive plates designed for the operation (or condylar blade plates) or external fixation with Hybrid or circular ring fixators. A combination of large K wires and prolonged cast immobilisation is a historical technique one may find detailed in the literature but of no merit compared to modern compressive fixation techniques.

GA or regional anaesthesia
Femoral & sciatic blocks for post-operative pain relief
Laminar flow , peri-operative antibiotics , 2-4 weeks of post operative LMW Heparin
Thigh tourniquet and Flowtron on contra-lateral calf
Ankle positioned into neutral using sandbags & side supports
Large , rolled up sterile towels behind the ankle to improve access for cuts.

2 weeks in back-slab
dressing changes at 1 & 2 weeks
Complete cast between weeks 2 to 6 & non-weight bear
Some compliant patients with good bone quality and good bone to bone contact at the arthrodesis site may be permitted to transfer into a post-operative boot either at the 2 week or 4 week stage and commence light weight-bearing. If other procedures have been required this is however precluded.
Check X-ray at 6 week stage . Usually may commence light weight bear and progress to 50% body weight by 12 weeks. Dependant upon age , bone quality and co-morbidities, either week
6-12 in a robust post-operative boot or in a walking cast.
Further X-ray at 12 weeks . Satisfactory progression is judged by both radiographic progression as well as a patients comfort upon limited weight-bearing.
Generally a further 6 weeks is required at this stage in a post-operative boot.The progression from partial to full weight -bearing is made during this period.
A further X-ray is performed at 18 weeks to confirm union and if symptoms are in keeping with this the patient may move onto a stiff-soled hiking boot for a further 4 weeks , then normal shoes.
No heavy manual type activity or sport for 5-6 months post operation.
Ultimately , normal shoe wear and activities as able. Following double fusion surgery however patients are more likely to require a shoe with a sole that approaches a traditional through-rocker , or require such a modification to a normal pair of shoes.

Tibiotalocalcaneal arthrodesis using a reamed retrograde locking nail.
Clin Orthop Rel Res 2007 Oct; 463 :151-6.
Boes R, Mader K , Pennig D , Verheyen CC.
50 patients were followed up for approximately 4 years. The ankle was formally prepared surgically and the Subtalar joint was not though all patients underwent reaming of both joints prior to nail insertion.
All ankles united with a mean time to union of 20 weeks , 2 Subtalar non-unions only. Patients were reviewed clinically and radiographically.
Surgical correction of severe deformity of the ankle and hindfoot by arthrodesis using a compressing retrograde intramedullary nail.
Foot Ankle Int 2014. 35 (4): 360-7.
Brodsky JW, Verschae G, Tenenbaum S.
30 cases followed for a mean of 30 months
Just under half of the patients had a deformity over 15 degrees varus or valgus coronal plane . 2/3rds were corrected to a deformity of less than 5 degrees. Union rate of over 96% reported. 10% temporary plantar nerve parasthesia, 10% wound infection and 10% developed a stress response.
Tibiotalocalcaneal arthrodesis with a curved ,interlocking ,intramedullary nail
Foot & Ankle Intl 2010. Dec ;(12):1085-92.
Budnar VM, Hepple S, Harries WG, Livingstone JA, Winson I.
45 fusions followed up for a mean of 4 years. Indications were for failed ankle fusion and replacement and complex ankle and hindfoot deformity. The nail design allowed for a lateral hindfoot insertion as opposed to plantar insertion.
Union rate was almost 90% , over 80% had reduced pain and 2/3rds of patients had improved function. 4 nails required removal
Tibiocalcaneal arthrodesis for the management of severe ankle and hindfoot deformities.
Foot & Ankle International.2000.21(8):643-649.
M.S.Myerson ,R.G.Alvarez ,P.W.C.Lam.
Condylar balde plate used for a mixture of pathologies ( including failed primary surgery and 8 cases of osteomyelitis) in 30 patients.
Nevertheless 28 went on to union at an average of 16 weeks.
Revision Tibiotalar arthrodesis.
J Bone and Joint Surg.2008.90-A:1212-1223.
M.E.Easley , H.E.Montijo ,J.B.Wilson ,R.D.Fitch ,J.A.Nunley.
45 patients reviewed who had undergone revision ( both primary revision and also 5 secondary revision cases).
External ring fixators used and overall 85% union rate
Reference
- orthoracle.com


































