Learn the Digital nerve repair: Autograft using medial cutaneous nerve of forearm surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Digital nerve repair: Autograft using medial cutaneous nerve of forearm surgical procedure.
Patients with nerve injuries sometimes present late due to a variety of reasons. Unlike a motor nerve where there is muscle atrophy after one year, a sensory nerve can have a delayed repair even years after the injury. Patients with unrepaired sensory nerves often have neuropathic pain from end neuroma along with loss of sensations.
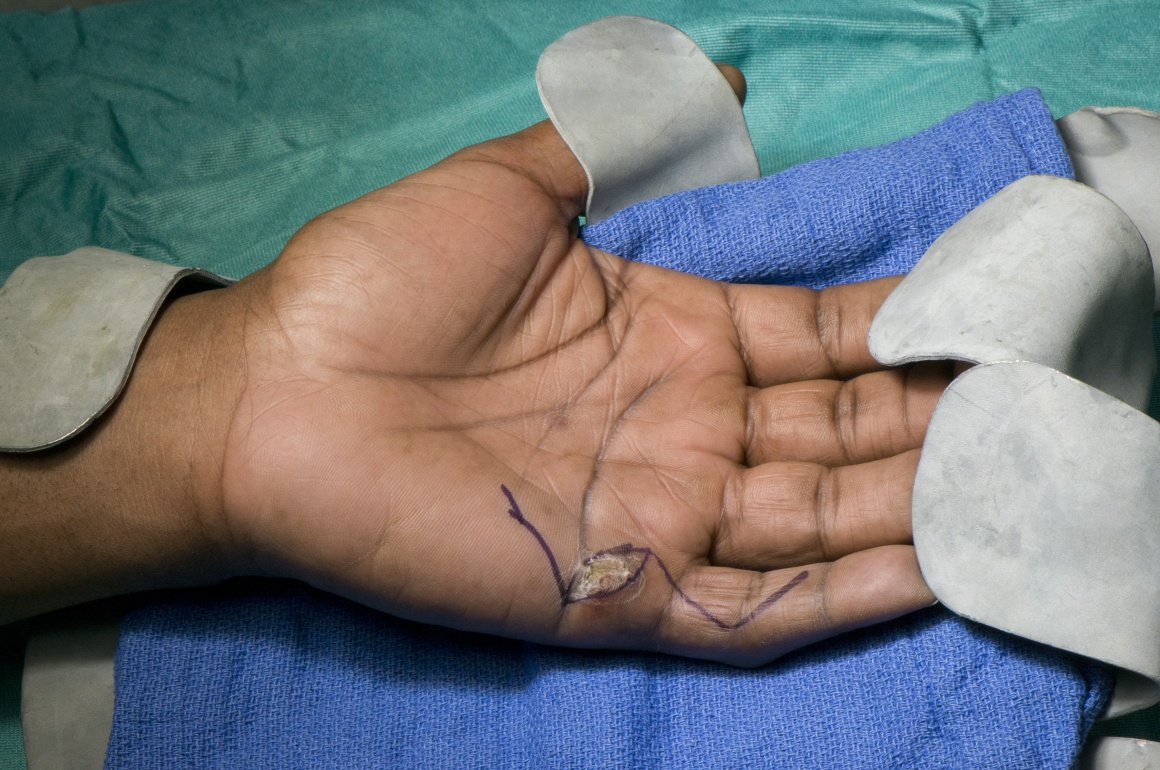
The patient discussed here had a glass laceration to his left hand four weeks ago. He was lost to follow up after the initial assessment and came back with a healed wound, inability to fully flex his little finger, loss of sensations along the ulnar side of the little finger and neuropathic pain. He had an X-Ray to rule out glass foreign bodies. The clinical diagnosis was of an injury to ulnar digital nerve of left little finger and a possible partial flexor tendon injury. The option of a nerve grafting was discussed with the patient. Though there are other options such as allografts and conduits, their use may be limited to gaps less than 3cm.
The donor nerve chosen in this case is the medial cutaneous nerve of the forearm which is a direct branch from the medial cord of the brachial plexus. The alternatives are sural nerve, lateral cutaneous nerve(which is a continuation of musculocutaneous nerve) or posterior interosseous nerve. Posterior interosseous nerve causes the least donor site morbidity but the length available is limited.
The main donor morbidity from the medial cutaneous nerve of the forearm is a patch of numbness in the medial aspect of the forearm. There is a small risk of a painful neuroma in the proximal stump of the donor nerve and for this reasons, most people bury it in the FCU muscle.

INDICATIONS:
The indication to explore a laceration or a healed laceration is loss of sensations of movements. With hand lacerations, most of them get formally explored in theatre. The mechanism of injury gives a clue to the depth of injury as glass lacerations tend to be deep. Commonly these injuries present acutely with lacerations to the hand. Clinical assessment includes a detailed history and examination. Points in history include age, hand dominance, occupation, hobbies, details of injury, disability such as loss of movements or numbness and past medical history. Smoking history is important as these patients should be advised to stop smoking in the post-operative period.
SYMPTOMS & EXAMINATION:
While examining an injured hand, one starts by assessing the location of the wounds which give a clue regarding the structures likely to be injured. With volar lacerations, one has to assess flexor tendons, nerves and circulations. With dorsal lacerations, extensor tendons need to be assessed. Though it is important to assess dorsal sensory nerve branches, these branches are small and seldom repairable. Circulation is assessed by checking colour, temperature, pulp turgor and capillary refill. Sensations are assessed by crude touch and by comparing with an uninjured finger. Two-point discriminations and monofilament testing are not practicable in the emergency setting. Flexor tendons are assessed separately for each digit and FDS and FDP and tested separately.
IMAGING:
X-Rays are done if bony injury is suspected or in the case of glass lacerations where one suspects a foreign body. In delayed presentations with healed wounds, ultrasound examination is useful to assess deep structures such as tendons and nerves and the level of injury.
ALTERNATIVE OPERATIVE TREATMENT:
When a nerve or tendon injury is suspected in a finger, surgical exploration and repair is indicated. Digital nerve injuries are more important in the thumb, index finger as well as the ulnar side of the little finger. With delayed presentations, digital nerve injuries in the central digits can sometimes be treated conservatively. There is a risk of neuroma formation in these cases and it may be worth trying to bury the proximal nerve stump into muscle or bone. When there is a gap in the digital nerve, autografts are the standard treatment options. Allograft(Avance® ;AxoGen, USA)is an also an option for these cases. NICE has approved the use of allograft for repair of digital nerve defects. These are available off the shelf in some hospitals. For critical areas such as thumb, radial side of index finger and ulnar side of little finger, I prefer to use autografts unless the patient has a preference not to have a nerve graft harvested.
The other alternatives are nerve conduits and autologous conduits such as free-thawed skeletal muscle and veins. There are several FDA approved commercially available nerve conduits including NeuraGen,® (Inegra Lifesciences, USA) Neurotube® (Synovis Microcompanies, USA), Neurolac™ (Polyganics, USA) and Axoguard®(AxoGen, USA). The limitation of the vein conduit is that it may collapse and does not allow the axonal regeneration. Freeze-thawed skeletal muscle has been tried on its own and in conjunction with veins but the results have not been encouraging.
Whilst allografts and conduits are attractive options the main limitation in their use is the gap which they can be used. At present nerve conduits are used for gaps up to 2omm. Allografts have been found to be effective in gaps up to 30mm.
NON-OPERATIVE MANAGEMENT:
Conservative treatment is an option for central digits which are not crucial for sensations. However there will be the risks or numbness and neuroma pain. When patients present with delayed injury and no neuroma pain, the merits of reconstruction should be weighed against the risk of donor site morbidity of nerve grafts and the risk of causing neuropathic pain.
CONTRAINDICATIONS:
Non-compliant patient. Infected wound.

Surgery is performed under a brachial block and tourniquet control. The hand and forearm is prepped and draped. The medial cutaneous nerve of the forearm has been chosen as the potential donor site for nerve graft. Sensory nerve usually follow the superficial veins. The surface marking for the branches of the medial cutaneous nerve of the forearm is the tributaries of the basilic vein. If the nerve is to be identified in the upper arm, the landmark is a point 2cm above and medial to the medial epicondyle. While doing sensory nerve repairs, a sheath of a superifical vein can be used to protect the repair site and it is planned for this case. One of the main advantages of using a vein sheath is that there is less risk of a neuroma tethering to the adjacent tissues and causing pain.
The surgical team has been instructed about the need for micro instruments and microscope. The initial dissection is done under loupe magnification and once the nerve ends are identified, microscope is brought in.

Patient is discharged home the same day.
Hand elevation in a sling is advised for 24 hours.
The rest of the post-op plan is as follows:
Wound dressing change: 1 week in Dressing clinic.
Redress with simple Mepore dressings. Patient is also referred to OTs to start mobilisation of wrist and fingers.
Removal of sutures: 2 weeks.
Patient is followed up at 4 weekly intervals monitoring for nerve recovery. Advancing Tinel’s sign approximately 1mm day is a sign of nerve recovery. Splinting following isolated digital nerve repair or grafting is not indicated. If there is an associated flexor tendon injury, splintage and therapy is guided by the protocol for flexor tendon repairs. In case of isolated digital nerve repairs, free movements are started from the first week. Normal activities of daily living can be resumed form two weeks. In case of manual workers, return to work and strenuous activities are deferred for six weeks. Scars tend to be tender in the palm and this improves between six to eight weeks. Patients are advised to massage the scars from the second week onwards.
Smokers tend to have poorer wound healing following hand injuries and they are advised to stop smoking in the post-operative period.
Assessment of outcomes are done when the time period for nerve recovery has elapsed. This is worked out by calculating the distance of the repair site from the tip of the digit, for example if it is 9 cm, the recovery should take about 90 days, or about 3 months. Patients are asked about their symptoms such as pain, cold intolerance as well as their ability to feel objects with the finger. Examination included testing for range of movements and tapping over the repair site for a static Tinel’s sign implying a neuroma. A subjective simple assessment is the Tens test wherein the patient is asked to rate the sensations out of 10, with 10 being that of a normal digit. More accurate assessments are done by measuring Two Point Discrimination and by testing using Semmes Weinstein monofilaments.
Complications of this procedure include common wound healing problems such as infection, wound break down and sensitive scars. Failure of nerve recovery and neuromas are specific problems in nerve surgery. In this case the pre-emptive use of vein sheaths help to minimise the risk of a painful neuroma.

Management of nerve gaps: autografts, allografts, nerve transfers, and end-to-side neurorrhaphy. Ray WZ, Mackinnon SE. Exp Neurol. 2010 May;223(1):77-85. This review article looks at the timing of nerve repairs including closed and open injuries, techniques of repairs and the management of nerve gaps. Techniques described include nerve transfers, autografts, conduits and allografts.
Outcomes of short-gap sensory nerve injuries reconstructed with processed nerve allografts from a multicenter registry study. Rinker BD, Ingari JV, Greenberg JA, Thayer WP, Safa B, Buncke GM. J Reconstr Microsurg. 2015 Jun;31(5):384-90. This study looked at a database(RANGER) evaluating patients who had digital nerve gaps managed using autografts and allografts. There were 24 patients in the study and it concluded that the outcomes were comparable between both groups.
Allograft reconstruction for digital nerve loss. Taras JS, Amin N, Patel N, McCabe LA. J Hand Surg Am. 2013 Oct;38(10):1965-71. This study looked at 21 digital nerve repairs in 17 patients where allograft was used for bridging nerve gaps. They concluded that allograft is appropriate for nerve repairs up to 30mm.
Reference
- orthoracle.com




































