Watch the overview
Learn the Dupuytrens contracture: Dermofasciectomy and skin grafting surgical technique with step by step instructions on OrthOracle. Our e-learning platform contains high resolution images and a certified CME of the Dupuytrens contracture: Dermofasciectomy and skin grafting surgical procedure.
Dupuytren’s disease is a fibroproliferative condition effecting palmar tissues of the hand resulting in contractures of the fingers. It has a genetic predisposition with a variable inheritance pattern. There are several environmental factors implicated in this condition including smoking, alcoholism, diabetes, and epileptic medications. Treatment of Dupuytren’s contractures is indicated mainly for contractures effecting hand function. The treatment is chosen based on several factors including whether it is a primary disease or recurrent; the degree of contracture; patient’s co-morbidities and patient preference.
Dupuytren’s disease is an inherited autosomal dominant trait with variable penetrance and expressivity. Normal fascia is composed mainly of type I collagen. In Dupuytren’s there is an increase of type III collagen (as also seen in wound healing) and myofibroblasts which are a contractile cell derivative from the fibroblast. With this contractile potential, the normal anatomical ‘Bands’ within the hand can become contracted ‘Cords’. In addition to ‘Cords’, ‘Nodules’ are seen when a bulk of Dupuytren’s tissue appears in one site and ‘Pits’ are seen when the skin fibers contract and pull small areas of skin down towards the deeper cords in the palm.
The recognised bands/cords are as follows:
Pretendinous band/cord– a continuation of the palmaris longus and palmar fascia which is in line with each digit and inserts around the flexor sheath at the level of the MCPJ crease (a central cord can continue in this line along the flexor sheath to the DIPJ).
Natatory ligament/cord– transverse cords which span between the web spaces blending with the pretendinous band/cord and spiral band/cord
Spiral band/cord– longitudinal structure superficial to neurovascular bundle (NVB) crossing from pretendinous band/cord to blend with lateral digital fascia, when contracted this pulls the lateral digital fascia/cord centrally and as the NVB is enclosed by Grayson’s and Cleland’s ligaments which are attached to the lateral digital fascia the NVB is then pully more centrally in the finger at the level of the MCPJ crease.
Lateral digital fascia/cord– longitudinal structure close to the skin running almost up the lateral midlines of the fingers attached to Grayson’s and Cleland’s ligaments.
Retrodigital fascia/cord – distal continuation of lateral digital fascia/cord which may cause DIPJ contracture.
Commisural band/cord– similar to Natatory but of the 1st web space
Legueu and Juvara septa/cord – vertical structures which separate the distal palm into sections with NVB and lumbrical then flexor sheaths in alternating sections.
Grapow fibre/cords– small vertical structures which tether the palmar skin to the deeper fascia and provide stability of the skin and cause pitting when contracted.
The treatment options for this condition include Needle aponeurotomy, Collagenase injection(though the drug has been currently withdrawn from the market), limited fasciectomy, segmental fasciectomy, and dermofasciectomy.
For a recurrent disease where there is the involvement of the skin, a Dermofasciectomy is recommended as it has the lowest recurrence rate. This procedure involves excising the segment of skin involved in Dupuytren’s disease and replacing it with a full-thickness skin graft from the forearm. This however carries a risk of graft loss in which case the wound has to be allowed to heal by secondary intention.
Adjunctive procedures apart from excision of the Dupuytren’s cords are sometimes required for these patients. When there is a contracture of the PIP joint which does not straighten by manipulation of the finger a sequential release of the joint can be attempted. This involves a release of the flexor sheath, release of the proximal attachment of the volar plate, and release of the accessory collateral ligaments. Release of the true collateral ligaments is not recommended as this causes instability and stiffness of the joint
With long-standing contractures of the PIP joint, the central slip may get attenuated resulting in a Boutnonnierre deformity. This is clinically seen as a flexed PIP joint and a hyperextended DIP joint. In these cases after the contractures are released with or without a joint release, full passive straightening is achieved but a tenodesis test(flexing the patient’s wrist extends the fingers suggesting the integrity of the tendon) will be negative. In these cases there may be a consideration for a central slip tightening procedure. This can be done by reattaching the attenuated central slip using a bone anchor or by doing a ‘Chamay’ incision and advancing the tendon proximally as can be seen in this case.
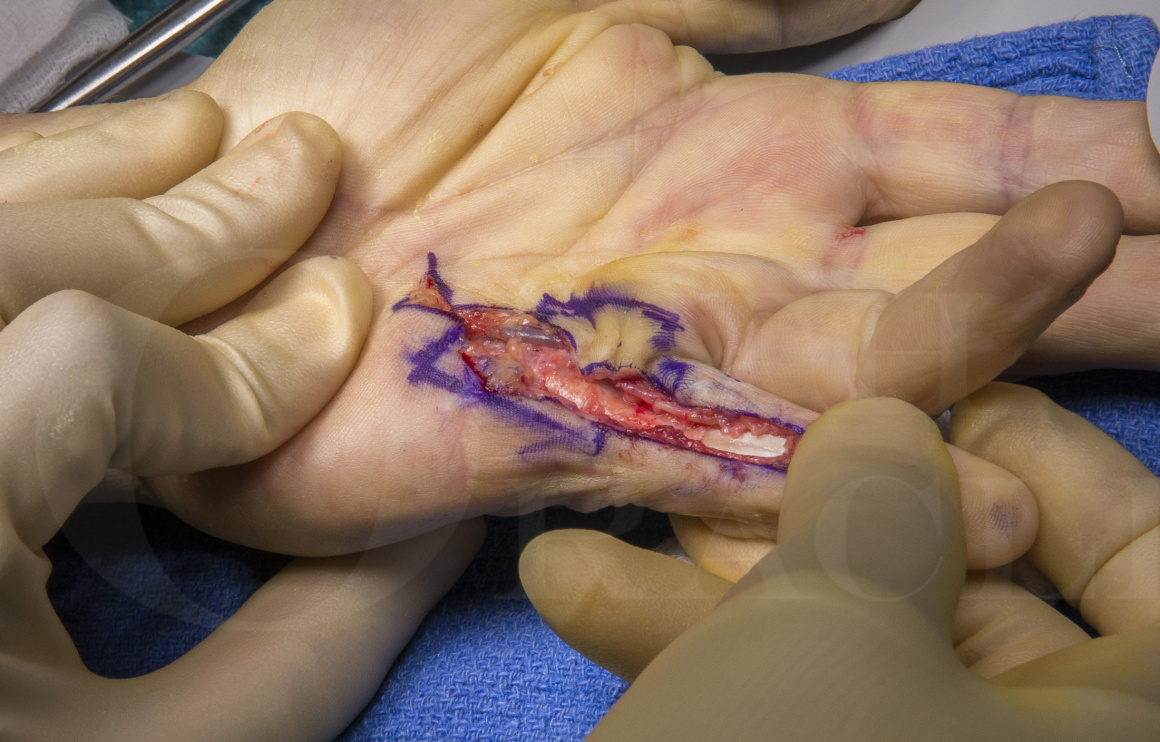
This case illustrates a recurrent Dupuytren’s disease affecting the left little finger in a middle-aged man. The primary procedure was a limited fasciectomy carried out 10years ago. There is noted recurrent disease and progression of the disease into the finger causing an MCP joint contracture of 30 degrees and a PIP joint contracture of 80 degrees. There is hyperextension of the DIP joint suggesting an attenuation of the central slip. The palmar skin is scarred and indurated suggesting its involvement by the disease. After a detailed discussion, a decision has been made to perform a dermofasciectomy with full-thickness skin grafting. The adjunctive procedures planned are PIP joint release and a central slip tightening.
Readers will also find the following OrthOracle techniques of interest:
Palmar and digital fasciectomy for Dupuytrens
Limited fasciectomy for Dupuytrens disease plus Z-plasties
Collagenase (Xiapex) injection and Manipulation for Dupuytrens contracture

Indications
A patient will present for treatment usually for one of three reasons:
1.They have lumps in the palm and are unsure of the diagnosis. These patients can be reassured based on a clinical diagnosis, educated on the condition, and discharged.
2.They are aware of the diagnosis and the tightness of the palm or nodules are a nuisance but no clear fixed flexion deformity – these patients are best educated about the condition and the likely recurrence rates and therefore avoidance of very early surgery to avoid scarring and increased future complications of repeat surgery. If they still would like intervention in specific cases (e.g. professional pianist whose span is reduced or tree surgeon with large nodules but no contracture making gripping difficult and climbing unsafe – reasonable surgical indications) they have two options in the UK. One is to have treatment in the private sector and the other is for the surgeon to apply for specific funding on individual grounds for the treatment to the funding body.
3.The patient has a contracture of the digit causing dysfunction. In the UK patients can undergo funded treatment for Dupuytren’s contractures based on certain guidelines. In the author’s region this states if there is a progressive PIPJ contracture or an MCPJ contracture of 30 degrees or more then treatment can proceed. These values are often the point at which dysfunction is increasing due to the contracture.
Symptoms
Dupuytren’s disease is a non-painful condition. Although the condition can be itchy or sore when active proliferation is taking place, or painful when gripping if large nodules are compressed, if pain is a main feature of the presentation then a rare but serious diagnosis of fibrosarcoma should be excluded.
Dupuytren’s contracture is a spectrum of severity and can range from a mild inconvenience to a disabling condition with all ten digits severely affected.
Patients complain of aching or cramping in the hands, a feeling of tightness, and the inconvenience of the contracted digit of poking then in the eye when washing their face, catching on their clothes when trying to get money out of their pocket, and sticking on door handle after they have opened them.
The Dupuytren’s diathesis is a collection of signs and conditions which are seen to suggest a worse prognosis in terms of disease progression and recurrence. This is made up of age <50, male, bilateral disease, radial-sided disease (thumb/index finger), family history, and ectopic disease. Ectopic sites include the dorsal PIPJ nodules (Garrod’s pads), penile fibrosis (Peyronie’s disease), plantar fibrosis (Lederhose’s disease).
Examination
The inspection usually reveals cords, nodules, and pits within the palms and fingers.
It should be noted from the history which specific fingers are troubling the patient, especially in the more severe disease when all fingers are affected and multiple treatments and recurrences have already occurred.
Joint contracture angles should be measured and recorded and it is useful to isolate each joint and record the combined and individual joint contractures. This is performed with a small finger goniometer on the dorsum of the finger. Initially, the whole finger is extended maximally and the joint angles recorded. Following this the MCPJ is fully flexed and PIPJ maximal extension is recorded then the PIPJ is maximally flexed and the MCPJ extension angle recorded.
This differential will help the surgeon identify if there is a spanning cord contracting both joints and help with prognosis to predict the postoperative correction.
As a general rule, all MCPJ contractures caused by Dupuytren’s no matter how severe will be corrected by treatment. Any PIPJ contracture above 60 degrees is likely to remain with some contracture post-treatment. This is due to the collateral ligament and volar plate contractures which can be released intra-operatively to provide a greater extension but at greater risk of joint stiffness, and loss of flexion.
After previous surgery a digital Allen’s test (as for Allen’s test at the wrist the finger can be squeezed by the examiner to exsanguinate and both digital arteries pressed upon and released one at a time first starting with Radial then on the second time starting with the Ulnar. The rate of reperfusion should be noted and if a significant difference noted between sides then a possibility of previous arterial injury should be considered) and assessment of sensation are also useful to record if further intervention is being planned.
Further examination of ectopic sites can be undertaken if necessary although usually only the dorsal PIPJ disease of Garrod’s pads is reviewed.
Investigations
There are no formal investigations for Dupuytren’s disease unless there is a concern regarding pain and a possible diagnosis of sarcoma. In this case a USS or MRI may be performed. This may also be necessary in an isolated nodule where diagnosis is unclear.
Non-operative Management
The best non-operative treatment is patient education and reassurance which includes advice on the stage of disease progression in which treatment is advised.
Non-operative management with splinting or physiotherapy has not shown to be effective. Radiotherapy is one option used to prevent disease progression however the evidence on its effectiveness is limited. The author does not use this in their treatment pathway.
Alternative operative Management
For primary disease involving MCP joint a needle aponeurotomy, collagenase injection, or a limited fasciectomy can all provide a good correction. However, the risks of the procedure and the recurrence rates vary.
Needle aponeurotomy: Low risk, recurrence rate up to 50%
Collagenase injection: Risks of skin tear and a very small risk of tendon injury, recurrence rate 30-40% Collagenase is currently not available in the market.
Limited fasciectomy: Risk of digital nerve injury(2%); recurrence rate 20-30%
It is important to note that recurrence rates do not equate to re-operation rates. The exact figures for re-operation for individual techniques are not available but are much less than the recurrence rates as many patients opt not to have a repeat operation and choose to accept the deformity.
Contraindications
A relative contraindication to a dermofasciectomy is multiple previous surgeries with rapid recurrence when alternative treatment options such as joint arthrodesis or amputation may be a better consideration.

This procedure can be performed under a Brachial block or General anesthesia. It is important to have a complete blockage of the arm if using a Brachial block to ensure that the area from where the skin graft is harvested is numb.
The procedure is carried out under loupe magnification.
The patient is in a supine position with the arm on a hand table. The surgeon and assistant sit down on either side of the arm.
As the procedure takes more than one hour, it is better to inflate the tourniquet just before making the incision to minimise the discomfort from the tourniquet.

The hand is elevated in a Bradford sling.
The patient is discharged home on the same day with oral analgesics.
The arm should be kept elevated during the post-operative period in a sling. The patient is advised not to use the hand for any activity.
The wound is checked in five days. The graft should be adherent to the wound with no discolouration.
A light dressing is applied and a hand based splint is made to keep the finger in extension for three weeks more. After that active flexion exercises are started and the splintage continued for the night time. The patient is advised to moisturise and massage the graft and the scars. After six weeks gentle passive exercised are started. This is continued for another six weeks. At the end of it patient should have regained flexion in the finger. The night splint may be discontinued if patient has a full active extension. The patient is followed up again at three months to check for any flexion deformity. There is any evidence of it night splintage is recommenced for another six weeks. The final review is done at six months.

1. Wade R, Igali L, Figus A. Skin involvement in Dupuytren’s disease. J Hand Surg Eur Vol. 2016;41(6):600-608.
This study looked at the skin histology of patients with Dupuytren’s disease. It was found that there was dermal involvement in 50% of patients undergoing fasciectomy and 70% of those undergoing dermofascietomy. Skin involvement was associated with greater pre-operative contracture, palmar nodules, and occupations involving manual labour. The authors hypothesised that skin has a greater role in the development of the disease than previously thought.
2. Ketchum LD. The use of the full thickness skin graft in Dupuytren’s contracture [published correction appears in Hand Clin 1992 May;8(2):followi]. Hand Clin. 1991;7(4):731-743.
This review article outlines the treatment options of Dupuytren’s disease including limited fasciectomy and dermofasciectomy. The role of dermofasicetomy and skin grafting is discussed with the benefit of low recurrence.
3. Ullah AS, Dias JJ, Bhowal B. Does a ‘firebreak’ full-thickness skin graft prevent recurrence after surgery for Dupuytren’s contracture?: a prospective, randomised trial. J Bone Joint Surg Br. 2009;91(3):374-378.
This is a randomised controlled trial which looked at the role of full-thickness skin grafts used as a fire break in minimising the risk of Dupuytren’s disease. These were patients who could have limited fasciectomy and skin closed without any problems. There was no significant difference between outcomes and the recurrence rate was 12.4%. It is important to note that these were not patients with recurrent disease and skin involvement.
Reference
- orthoracle.com


































































